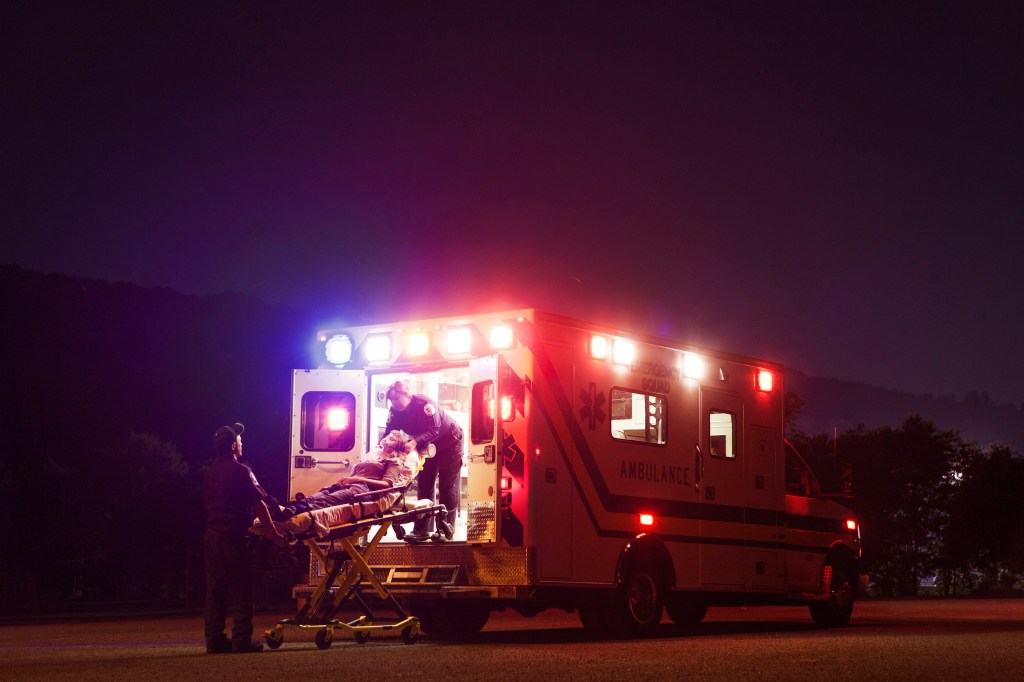
California Health Workers May Face Rude Awakening With $25 Minimum Wage Law
SACRAMENTO, Calif.
— Nearly a half-million health workers who stand to benefit from California’s nation-leading $25 minimum wage law could be in for a rude awakening if hospitals and other health care providers follow through on potential cuts to hours and benefits.
A medical industry challenge to a new minimum wage ordinance in one Southern California city suggests layoffs and reductions in hours and benefits, including cuts to premium pay and vacation time, could be one result of a state law set to begin phasing in in June. However, some experts are skeptical of that possibility.
The California Hospital Association brought a partly successful legal challenge to Inglewood’s $25 minimum wage ordinance, which barred employers from taking those sorts of steps to offset their higher costs.
“Layoffs, reductions in premium pay rates, reductions in non-wage benefits, reductions in hours, and increased charges are consequences of an employer having less money to spend—which will necessarily be the case given the significant increase in spending on wages due to the minimum wage,” the association said in its lawsuit. Additional examples include reducing health coverage and charging for parking or work-related equipment.
Inglewood voters approved the ordinance in November 2022, nearly a year before California legislators enacted a $25 minimum wage for health workers. Those statewide higher wages are to be phased in starting in June under California’s first-in-the-nation law, but Gov. Gavin Newsom has since said they are too expensive as the state faces a deficit estimated between $38 billion and $73 billion. It’s unclear if lawmakers will agree to a delay or take other steps to reduce the cost.
U.S. District Judge Dale S. Fischer agreed with the hospital industry in a March 11 tentative ruling when he shot down the portion of Inglewood’s ordinance banning layoffs and clawbacks by employers, while allowing the rest of the ordinance to remain in effect. He gave the sides time to object to his preliminary decision, though none did.
The California Hospital Association represents more than 400 hospitals and was a key backer of the state’s carefully crafted compromise law, which notably contains none of the employee safeguards included in the Inglewood ordinance.
Spokesperson Jan Emerson-Shea said the association doesn’t know how providers will react once the state law takes effect. “We don’t have any insights,” she said.
“The challenge for any health care organization is figuring out how to pay for the higher wages,” said Joanne Spetz, director of the Philip R. Lee Institute for Health Policy Studies at the University of California-San Francisco. “Since labor costs are the largest part of any health care organization’s costs, it’s hard to figure out how to reduce spending without looking at labor costs.”
Providers can try to increase revenues by bargaining for higher reimbursements from commercial insurers, she said. Public hospitals, nursing homes, and community clinics get most of their money through Medi-Cal, the state’s Medicaid program.
Providers could reduce the services they offer, pare back charity care, and cut or delay capital investments, Spetz said. In the long term, she expects some combination of spending cuts and revenue increases.
Both the state law and local ordinance cover far more than doctors and nurses, with a definition of health worker that includes janitors, housekeepers, groundskeepers, security guards, food service workers, laundry workers, and clerical staff.
The most recent estimate by the Health Care Program at the University of California-Berkeley Labor Center is that as many as 426,000 health workers would make an average of $6,400 extra in the law’s first year, a 19% average pay bump mainly benefiting lower-income workers of color and women. State finance officials project that well over 500,000 workers will benefit.
Researchers didn’t include layoffs and other potential staffing and benefit reductions when they projected the state law’s costs and benefits, said Laurel Lucia, the program’s director. But she pointed to initial projections by hospitals, doctors, and business and taxpayer groups that the wage hike would cost $8 billion annually, thereby imperiling services and resulting in higher premiums and higher costs for state and local governments.
“It seems like a contradiction to say this law’s going to cost billions of dollars while at the same time saying it’s going to reduce workers’ total compensation,” said Lucia, who projects a far lower price tag.
She added that state finance officials had anticipated that Medi-Cal reimbursements would reflect the increased labor costs, while Medicare would eventually at least partially compensate for the higher labor costs.
Michael Reich, chair of the Center on Wage and Employment Dynamics at UC Berkeley’s Institute for Research on Labor and Employment, and affiliated economist Justin Wiltshire recently argued that California’s new $20 minimum wage law for fast-food workers won’t result in mass layoffs and price increases, as some have predicted.
Health care is much different than fast food, Reich acknowledged, but he argued for much the same positive result.
“A higher minimum wage will make it easier and cheaper for hospitals to recruit and retain these workers. The cost savings, and the productivity benefits of more experienced workers, could offset much of the labor cost increase,” Reich said.
The hospital association filed its lawsuit against Inglewood’s ordinance in July, while it was still opposing early versions of the statewide minimum wage legislation. Among many other provisions, the statewide law put on hold an initiative to cap hospital executives’ salaries in Los Angeles.
The hospital association’s legal challenge referenced in part layoffs and reduced working hours imposed by Centinela Hospital Medical Center after Inglewood’s ordinance took effect.
But Centinela said the reduction was entirely unrelated to the ordinance and that all staff were offered alternate positions, which many accepted.
“Centinela Hospital also has since added many more jobs in new clinical positions above minimum wage scale,” the hospital said in a statement.
Service Employees International Union-United Healthcare Workers West, the prime backer of both the local ordinance and the statewide law, sued the hospital in April 2023 alleging that it cut workers’ hours to offset the higher minimum wage. The case is still pending.
The union did not respond to repeated requests for comment.
In a court filing, however, the union and city of Inglewood said similar employer restrictions in previous minimum wage laws have survived.
The ordinance “merely sets the backdrop for collective bargaining negotiations,” and does not bar employers from locking out employees or hiring replacement workers during a strike. Employers can still lay off workers or reduce their hours, they said, so long as they don’t do so to fund the higher minimum wage.
But Fischer agreed with the hospital association that layoffs and reductions in employees’ total compensation packages are “obvious responses by an employer to rising compensation costs.”
Restricting employers’ options would violate federal labor relations rules, he said.
“The minimum wage an employer has to pay its employees will invariably affect the total amount of compensation it is able or willing to pay,” he wrote “This will then invariably affect the number of employees it can retain and the number of hours those employees will be scheduled to work.”
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 3 months ago
california, Health Industry, States, Cost of Living, Hospitals, Legislation
What the Health Care Sector Was Selling at the J.P. Morgan Confab
SAN FRANCISCO — Every year, thousands of bankers, venture capitalists, private equity investors, and other moneybags flock to San Francisco’s Union Square to pursue deals. Scores of security guards keep the homeless, the snoops, and the patent-stealers at bay, while the dealmakers pack into the cramped Westin St.
Francis hotel and its surrounds to meet with cash-hungry executives from biotech and other health care companies. After a few years of pandemic slack, the 2024 J.P. Morgan Healthcare Conference regained its full vigor, drawing 8,304 attendees in early January to talk science, medicine, and, especially, money.
1. Artificial Intelligence: Revolutionary or Not?
Of the 624 companies that pitched at the four-day conference, the biggest overflow crowd may have belonged to Nvidia, which unlike the others isn’t a health care company. Nvidia makes the silicon chips whose computing power, when paired with ginormous catalogs of genes, proteins, chemical sequences, and other data, will “revolutionize” drug-making, according to Kimberly Powell, the company’s vice president of health care. Soon, she said, computers will customize drugs as “health care becomes a technology industry.” One might think that such advances could save money, but Powell’s emphasis was on their potential for wealth creation. “The world’s first trillion-dollar drug company is out there somewhere,” she dreamily opined.
Some health care systems are also hyping AI. The Mayo Clinic, for example, highlighted AI’s capacity to improve the accuracy of patient diagnoses. The nonprofit hospital system presented an electrocardiogram algorithm that can predict atrial fibrillation three months before an official diagnosis; another Mayo AI model can detect pancreatic cancer on scans earlier than a provider could, said Matthew Callstrom, chair of radiology at the Mayo Clinic in Rochester, Minnesota.
No one really knows how far — or where — AI will take health care, but Nvidia’s recently announced $100 million deal with Amgen, which has access to 500 million human genomes, made some conference attendees uneasy. If Big Pharma can discover its own drugs, “biotech will disappear,” said Sherif Hanala of Seqens, a contract drug manufacturing company, during a lunch-table chat with KFF Health News and others. Others shrugged off that notion. The first AI algorithms beat clinicians at analyzing radiological scans in 2014. But since that year, “I haven’t seen a single AI company partner with pharma and complete a phase I human clinical trial,” said Alex Zhavoronkov, founder and CEO of Insilico Medicine — one of the companies using AI to do drug development. “Biology is hard.”
2. Weight Loss Pill Profits and Doubts
With predictions of a $100 billion annual market for GLP-1 agonists, the new class of weight loss drugs, many investors were asking their favorite biotech entrepreneurs whether they had a new Ozempic or Mounjaro in the wings this year, Zhavoronkov noted. In response, he opened his parlays with investors by saying, “I have a very cool product that helps you lose weight and gain muscle.” Then he would hand the person a pair of Insilico Medicine-embossed bicycle racing gloves.
More conventional discussions about the GLP-1s focused on how insurance will cover the current $13,000 annual cost for the estimated 40% of Americans who are obese and might want to go on the drugs. Sarah Emond, president of the Institute for Clinical and Economic Review, which calculates the cost and effectiveness of medical treatments, said that in the United Kingdom the National Health Service began paying in 2022 for obese patients to receive two years of semaglutide — something neither Medicare nor many insurers are covering in the U.S. even now.
But studies show people who go off the drugs typically regain two-thirds of what they lose, said Diana Thiara, medical director for the University of California-San Francisco weight management program. Recent research shows that the use of these drugs for three years reduces the risk of death, heart attack, and stroke in non-diabetic overweight patients. To do right by them, the U.S. health care system will have to reckon with the need for long-term use, she said. “I’ve never heard an insurer say, ‘After two years of treating this diabetes, I hope you’re finished,’” she said. “Is there a bias against those with obesity?”
3. Spotlight on Tax-Exempt Hospitals
Nonprofit hospitals showed off their investment appeal at the conference. Fifteen health systems representing major players across the country touted their value and the audience was intrigued: When headliners like the Mayo Clinic and the Cleveland Clinic took the stage, chairs were filled, and late arrivals crowded in the back of the room.
These hospitals, which are supposed to provide community benefits in exchange for not paying taxes, were eager to demonstrate financial stability and showcase money-making mechanisms besides patient care — they call it “revenue diversification.” PowerPoints skimmed through recent operating losses and lingered on the hospital systems’ vast cash reserves, expansion plans, and for-profit partnerships to commercialize research discoveries.
At Mass General Brigham, such research has led to the development of 36 drugs currently in clinical trials, according to the hospital’s presentation. The Boston-based health system, which has $4 billion in committed research funding, said its findings have led to the formation of more than 300 companies in the past decade.
Hospital executives thanked existing bondholders and welcomed new investors.
“For those of you who hold our debt, taxable and tax-exempt, thank you,” John Mordach, chief financial officer of Jefferson Health, a health system in Pennsylvania and New Jersey. “For those who don’t, I think we’re a great, undervalued investment, and we get a great return.”
Other nonprofit hospitals talked up institutes to draw new patients and expand into lucrative territories. Sutter Health, based in California, said it plans to add 30 facilities in attractive markets across Northern California in the next three years. It expanded to the Central Coast in October after acquiring the Sansum Clinic.
4. Money From New — And Old — Treatments for Autoimmune Disease
Autoimmunity drugs, which earn the industry $200 billion globally each year, were another hot theme, with various companies talking up development programs aimed at using current cancer drug platforms to create remedies for conditions like lupus and rheumatoid arthritis. AbbVie, which has led the sector with its $200 billion Humira, the world’s best-selling drug, had pride of place at the conference with a presentation in the hotel’s 10,000-square-foot Grand Ballroom.
President Robert Michael crowed about the company’s newer autoimmune drugs, Skyrizi and Rinvoq, and bragged that sales of two-decades-old Humira were going “better than anticipated.” Although nine biosimilar — essentially, generic — versions of the drug, adalimumab, entered the market last year, AbbVie expects to earn more than $7 billion on Humira this year since the “vast majority” of patients will remain on the market leader.
In its own presentation, biosimilar-maker Coherus BioSciences conceded that sales of Yusimry, its Humira knockoff listed at one-seventh the price of the original, would be flat until 2025, when Medicare changes take effect that could push health plans toward using cheaper drugs.
Biosimilars could save the U.S. health care system $100 billion a year, said Stefan Glombitza, CEO of Munich-based Formycon, another biosimilar-maker, but there are challenges since each biosimilar costs $150 million to $250 million to develop. Seeing nine companies enter the market to challenge Humira “was shocking,” he said. “I don’t think this will happen again.”
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 6 months ago
california, Health Industry, Pharmaceuticals, States, Health IT, Hospitals, Prescription Drugs
KFF Health News' 'What the Health?': New Year, Same Abortion Debate
The Host
Julie Rovner
KFF Health News
Julie Rovner is chief Washington correspondent and host of KFF Health News’ weekly health policy news podcast, “What the Health?” A noted expert on health policy issues, Julie is the author of the critically praised reference book “Health Care Politics and Policy A to Z,” now in its third edition.
It’s a new year, but the abortion debate is raging like it’s 2023, with a new federal appeals court ruling that doctors in Texas don’t have to provide abortions in medical emergencies, despite a federal requirement to the contrary. The case, similar to one in Idaho, is almost certainly headed for the Supreme Court. Meanwhile, Congress returns to Washington with only days to avert a government shutdown by passing either full-year or temporary spending bills. And with almost no progress toward a spending deal since the last temporary bill passed in November, this time a shutdown might well happen.
This week’s panelists are Julie Rovner of KFF Health News, Lauren Weber of The Washington Post, Shefali Luthra of The 19th, and Victoria Knight of Axios.
Panelists
Victoria Knight
Axios
Shefali Luthra
The 19th
Lauren Weber
The Washington Post
Among the takeaways from this week’s episode:
- New year, same Congress. It’s likely lawmakers will fall short of their early-year goals to pass necessary spending bills, prompting another government shutdown or yet another short-term extension. And funding for pediatric medical training is among the latest casualties of the clash over gender-affirming care, raising the odds of a political fight over the federal health budget.
- The emergency abortion care decision out of Texas this week underscores the difficult position health care providers are in: Now, a doctor could be brought up on charges in Texas for performing an abortion in a medical emergency — or brought up on federal charges if they abstain.
- A new law in California makes it easier for out-of-state doctors to receive reproductive health training there, a change that could benefit medical residents in the 18 states where it is effectively impossible to be trained to perform an abortion. But some doctors say they still fear breaking another state’s laws.
- Another study raises questions about the quality of care at hospitals purchased by private equity firms, an issue that has drawn the Biden administration’s attention. From the Journal of the American Medical Association, new findings show that those private equity-owned hospitals experienced a 25% increase in adverse patient events from three years before they were purchased to three years after.
- And “This Week in Medical Misinformation”: Robert F. Kennedy Jr. earned PolitiFact’s 2023 Lie of the Year designation for his “campaign of conspiracy theories.” The anti-vaccination message he espouses has been around a while, but the movement is gaining political traction — including in statehouses, where more candidates who share RFK Jr.’s views are winning elections.
Also this week, Rovner interviews Sandro Galea, dean of the Boston University School of Public Health, about how public health can regain the public’s trust.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: Politico’s “Why Democrats Can’t Rely on Abortion Ballot Initiatives to Help Them Win,” by Alice Miranda Ollstein, Jessica Piper, and Madison Fernandez.
Lauren Weber: The Washington Post’s “Can the Exhausted, Angry People of Ottawa County Learn to Live Together?” by Greg Jaffe.
Victoria Knight: Politico’s “Georgia Offered Medicaid With a Work Requirement. Few Have Signed Up.” by Megan Messerly and Robert King.
Shefali Luthra: Stat News’ “Medical Marijuana Companies Are Using Pharma’s Sales Tactics With Little of the Same Scrutiny,” by Nicholas Florko.
Also mentioned in this week’s episode:
- Law Dork’s “ADF Is Providing Free Legal Representation to Idaho in Anti-Abortion, Anti-Trans Cases,” by Chris Geidner.
- JAMA Network Open’s “Barriers to Family Building Among Physicians and Medical Students,” by Zoe King, Qiang Zhang, Jane Liang, et al.
- The Journal of the American Medical Association’s “Changes in Hospital Adverse Events and Patient Outcomes Associated With Private Equity Acquisition,” by Sneha Kannan, Joseph Dov Bruch, and Zirui Song.
- KFF Health News’ “RFK Jr.’s Campaign of Conspiracy Theories Is PolitiFact’s 2023 Lie of the Year,” by Madison Czopek, PolitiFact, and Katie Sanders, PolitiFact.
click to open the transcript
Transcript: New Year, Same Abortion Debate
KFF Health News’ ‘What the Health?’Episode Title: New Year, Same Abortion DebateEpisode Number: 328Published: Jan. 4, 2024
[Editor’s note: This transcript was generated using both transcription software and a human’s light touch. It has been edited for style and clarity.]
Julie Rovner: Hello, Happy New Year, and welcome back to “What the Health?” I’m Julie Rovner, chief Washington correspondent for KFF Health News. And I’m joined by some of the best and smartest health reporters in Washington. We’re taping this week on Thursday, Jan. 4, at 10 a.m. As always, news happens fast, and things might have changed by the time you hear this, so here we go. Today we are joined via video conference by Lauren Weber of The Washington Post.
Lauren Weber: Hello, hello.
Rovner: Victoria Knight of Axios News.
Victoria Knight: Hey, everyone.
Rovner: And Shefali Luthra of The 19th.
Shefali Luthra: Hello.
Rovner: An entire panel of KFF Health News alums. I’m pretty sure that is a first. Later in this episode, we’ll have my interview with Boston University School of Public Health dean Dr. Sandro Galea. He has a new and pretty provocative prescription for how public health can regain public trust. But first, there was plenty of news over the holiday break, in addition to my Michigan Wolverines going to the national championship — sorry, Lauren — plenty of health news, that is. So we shall get to it. We will start on Capitol Hill, where Congress is poised to come back into session — apparently no closer to a deal on the appropriations bills that keep the government open than they were when they left for Christmas, and now it’s only two weeks until the latest continuing resolution ends. Victoria, are we looking at a shutdown again?
Knight: I was texting a lot of people yesterday trying to feel out the vibes. I think a lot of people think a shutdown seems pretty likely. A reminder that we have another member of Congress that is leaving on the Republican side in the House, so now the Republicans can only lose two votes if they’re trying to pass a bill. So when you have House Freedom Caucus members saying, “Hey, we don’t want to agree to any appropriations bills without doing something about the border,” and Democrats unlikely to agree to any border demands that the Freedom Caucus is wanting, it seems like we may be at a standstill. I know there is some reporting this morning that possibly they may just do another fiscal year continuing resolution until …
Rovner: You mean like the last couple of years we’ve done a full-year CR?
Knight: Yeah, exactly. So …
Rovner: The thing they swore they wouldn’t do.
Knight: And [House] Speaker [Mike] Johnson said, he promised he wouldn’t do that, so it’ll be interesting to see how that all plays out. As far as I’ve heard the latest, there’s no top-line funding number, but it does seem like a shutdown may be looming.
Rovner: Well, assuming there is a spending deal at some point, and the fact that 2024 is an election year where not much gets passed, a lot of lawmakers have a lot of things they would like to attach to a moving spending train, assuming there is a moving spending train. What’s the outlook for the bill that we were talking about all of December on PBMs [pharmacy benefit managers] and health transparency and some extensions of some expiring programs That’s still kicking around, right?
Knight: Yeah. That’s definitely still kicking around. So there are some extenders like for community health centers and averting some cuts to safety-net hospitals. Those are really high priority for lawmakers. I think those will make their way onto any kind of deal most likely. What seems more up in the air is the transparency measures for PBMs and for hospitals and for insurers. That was the big, as you mentioned, the big pass the House in December. The Senate has introduced their own versions of the bill and there’s talk that maybe some of that could ride onto if there is some kind of funding deal, but it’s also possible that maybe it’s more likely to be punted to the lame duck session. So, post-election, when Republicans are trying in the House and Senate Democrats are trying to do their last hurrah before the new Congress comes in. So we’ll see. Latest I heard yesterday there were some negotiations around the transparency stuff, so it’s still possible, but who knows?
Rovner: Congress is the ultimate college student. They don’t do anything until they have a deadline. Meanwhile, we have yet another health program caught up in the culture wars, this time the Children’s Hospital Graduate Medical Education [Payment] program. Because most medical residencies are funded by Medicare and because Medicare doesn’t have a lot of patients in children’s hospitals, this program was created in 1999 to remedy that. Yes, I covered it at the time. Republicans in the House are happy to reauthorize it or just to fund it through the appropriations process, which keeps the money flowing, but only if it bans funding for children’s hospitals that don’t provide gender-affirming care for transgender minors. It appears that has killed the reauthorization bill that was moving for this year. Is that the kind of thing that could also threaten the HHS [Department of Health and Human Services] spending bill?
Knight: Yeah, I mean there are provisions within the HHS bill to ban Medicare, Medicaid paying for gender-affirming care. I don’t know. We haven’t done much debate on the Labor-HHS bill. It’s been the one that’s been put to the side. It hasn’t even gone through the full committee, so we haven’t …
Rovner: In the House, right?
Knight: Yeah, in the House, yes. Yeah. But yeah, I think it’s definitely possible. Just broader picture, this is an issue that Republicans are trying to make a bigger thing that they’re running on in different congressional districts, talking about banning gender-affirming care. So I think even if we don’t see it now, it’s probably something that we’re going to continue seeing.
Rovner: Well, we will obviously talk more as Congress comes back and tries to do things. So new year, same old abortion debate. This week’s big entry is a decision by a panel of the 5th Circuit Court of Appeals ruling that EMTALA, the federal law that requires hospitals to at least screen and provide stabilizing care to anyone who presents in their emergency room, does not supersede Texas’ abortion ban. In other words, if a pregnant woman needs an abortion to stabilize her condition, she’d also have to meet one of the exceptions in the Texas abortion ban. Given that we don’t really know what the Texas exceptions are, since we’ve had litigation on that, that could be a tall order, right, Shefali?
Luthra: Yes. Doctors have basically said that the Texas exceptions in the state law are unworkable. And I think it’s worth noting that what EMTALA would require and what is in effect in other states with abortion bans is again very narrow. We are talking about the smallest subset of abortions, the smallest subset of medical emergency abortions, because this doesn’t apply to someone with a fetal anomaly who cannot give birth to a viable child. This doesn’t apply to someone who maybe is undergoing chemotherapy and can’t stay pregnant. This is for people who have situations such as sepsis or preterm premature membrane rupture. These are really, really specific instances, and even then, Texas is arguing and the 5th Circuit says, hospitals don’t have to provide care that would by all accounts be lifesaving.
Rovner: This puts doctors, particularly in Texas, in an untenable situation where if a woman presents, say, with an ectopic pregnancy, which is neither going to produce a live baby and is likely or could definitely kill the woman, if they perform that abortion, they could be brought up on charges in Texas, but if they don’t perform the abortion, they could be brought up on federal charges.
Luthra: And this is the bind that doctors have found themselves in over and over again. And I do want to reiterate that this isn’t actually unique to Texas because even in states where the EMTALA guidance is in effect, doctors and hospitals remain very afraid of coming up against the very onerous abortion penalties that their laws have. I was talking to a physician from Tennessee earlier this week, and she made the point that what your doctor feels safe doing, it comes down to luck in a lot of ways. Which city you happen to live in, which hospital you happen to go to, what the lawyers on that hospital staff happen to think the law says. It’s really untenable for physicians, for hospitals, and more than anyone else for patients.
Rovner: Now, despite Justice [Samuel] Alito’s hope in his Dobbs opinion overturning Roe that the Supreme Court would no longer have to adjudicate this issue, that’s exactly what’s going to happen. There’s already an emergency petition at SCOTUS from Idaho wanting to reverse a 9th Circuit ruling, preventing them from enforcing their abortion ban over EMTALA. In other words, the 9th Circuit basically said, no, we’re going to put this Idaho ban on hold to the extent that it conflicts with EMTALA until it’s all the way through the courts. Not to mention the mifepristone case that could roll back availability of the abortion pill. Is it fair to say that Justice Alito’s reasoning backfired here, or was he being disingenuous when he … did he know this was going to come back to the court?
Luthra: Not one of us can see inside any individual justice’s heart or mind, but I think we can say that anyone who seriously thought that overturning Roe v. Wade, which had been in effect for almost 50 years, would bring up no legal questions to be answered again and again by the courts clearly hadn’t thought this through. I was talking to scholars this week who think that we’ll be spending the next decade answering through the courts all of the new questions that have been instigated by the decision.
Rovner: Yeah, that’s definitely not going to lower their workload. Well, speaking of Idaho, the “Law Dork” blog has an interesting story this week about how the Alliance Defending Freedom — it’s a self-identified Christian law firm that represents mostly anti-abortion and other conservative groups in court — is now providing free representation to the state of Idaho in its effort to keep its state abortion ban in place. ADF is also representing Idaho in a case about bathroom use by transgender people. Now, conservative organizations and states often work together on cases, as do liberal organizations in states, that is not rare. But in this case, ADF is actually representing the state, which poses all kinds of conflicts-of-interest questions, right? Lauren, you’re nodding.
Weber: Yeah, I mean it’s pretty wild to see this kind of overlap. As you pointed out, Julie, it’s not rare for attorney general’s offices to seek outside legal help, that happens all the time. They’re understaffed. There’s a lot of problems they can address. But to fully turn over a case essentially to an ideological group is something different altogether because it also implies that that group is giving a gift to the government. It implies that they may be able to take on more cases because if it’s for free, then who knows? And I want to point out that this group really is at the forefront of many of the battles that we’re seeing play out in health issues legally across the country. I mean, they’re involved in a lot of the gender-affirming care cases and even in dealing with some of the groups that are promoting some of the legislation in places across the country. So this is quite a novel step and something to definitely be on the lookout for as we pay attention to many court cases that are going to play out over the next couple of years.
Rovner: Yeah, this was something I hadn’t really focused on until I saw this story and I was like, “Oh, that is a little bit different from what we’ve seen.” Well, while we were on the subject of doctors and lawsuits and the 5th Circuit Court of Appeals, a panel there kept alive a case filed by three doctors against the FDA, charging that it overstepped its authority by recommending that doctors not prescribe ivermectin, an anti-parasite drug, for covid. We’ve talked a lot about how the mifepristone case could undermine FDA’s drug approval process. Obviously, if anyone can sue to effectively get a drug approval reversed, this case could basically stop the FDA from telling the public about evidence-based research, couldn’t it?
Weber: This case is quite wild. I mean, as someone that covers misinformation and disinformation and has extensively covered the ivermectin sagas over the last couple of years, the idea that the FDA cannot come out and say, “Look, this drug is not recommended,” it would be a severe restricting of its authority. I mean, government agencies are known to give advice, which does not always have to be neutral. Historically, that is what has been considered just the status quo legally. And so for the court to restrict the FDA’s authority in this way — if this does, it’s obviously still up for appeal, so who knows? But if it were to be successful, essentially everything the FDA ever put out would have to say, “But go talk to your physician,” which would lead to a little bit more of a wild, wild West when it comes to evidence-based medicine as we know it today.
Rovner: Back on the abortion beat, the news isn’t all about bans in California. The new year is bringing several new laws aimed at making abortion easier to access. Shefali, tell us about some of those.
Luthra: California is really interesting because they really position themselves as the antithesis of states banning abortion. And the law that you’re discussing here, Julie, this is part of a real concern that a lot of physicians have, which is that in states with abortion bans, it’ll be harder for medical residents to be trained in appropriate health care. That means providing abortion care. It means providing comprehensive OB-GYN care in general, right? Miscarriage management, you learn how to do that in part by providing abortions. California has implemented a law this year that would try to help more out-of-state doctors come to California to get trained in how to provide this kind of care.
I think where this gets tricky and where doctors I’ve spoken to remain concerned, confused, it’s not a panacea, is the concern about whether any single state in and of itself can do enough to rectify what is happening in 18 states across the country. That’s a very, very tall order, and it comes with other concerns of: Will residents feel safe, able to come to California? Will their institutions want to send them? These are all open questions, and I think this California law, this project that they’re taking on, is incredibly interesting. I think it’ll take some time for us to see both what the impact is and what the kinks and challenges are that emerge along the way.
Rovner: I was also interested in a California law that says that California officials don’t have to cooperate with out-of-state investigations into doctors prescribing abortion pills or gender-affirming care.
Luthra: This is, again, really interesting, and I mean, I think what we are going to see is individual state laws continuing to run up against each other and questions over whose authority applies in what situations. This has come up for doctors constantly, right? The ones who live in states with abortion protections but want to provide care in other states. What happens if they are flying across the country and have a layover in a state with an abortion ban? What happens if they have a medical emergency in a state that they have maybe broken the law of, whose law applies there? These are things that have left a lot of doctors really concerned. I know I’ve spoken to physicians who say that even despite the legal protections in their states, in a state like California for instance, they still don’t feel safe actively breaking another state’s laws. And again, this is just one of those questions we’re going to keep watching and seeing play out. Who ultimately is able to decide what happens and what role would the federal government eventually have to play?
Rovner: I think these were things, these were the kinds of questions that I don’t think the Supreme Court really considered when they overturned Roe. There’s so many ramifications that we just didn’t expect. I mean, there were some that we did, but this seems to be an extent that it’s gone to that was not anticipated.
Luthra: It’s just a whole mess of, if not undesired, then perhaps unanticipated or not fully planned-for questions and concerns that are now emerging.
Rovner: So I wanted to call out a survey in the Journal of the American Medical Association about reproduction more broadly, not about abortion. How hard it is for medical students and young doctors to build families early in their careers — a time when most people are building their families. Medical training takes so long in many cases that women, in particular, may find it much more difficult or impossible to get pregnant if they wait until after their training is done. And the pace of medical care delivery and the patriarchal structure of most medical practice frowns on women doing things like getting pregnant and having babies and trying to raise children. I vividly remember a doctor retreat I spoke at in 2004 when a 30-something OB-GYN said that when she got pregnant, her residency adviser accused her of wasting a residency spot that could have gone to someone who wasn’t going to take time out of their career. I think things have progressed since then, but apparently not all that much, according to this survey.
Luthra: And this, I think, is really interesting because especially after the covid pandemic, we saw obviously, health care workers leave the field in droves. We saw more women leave the field than men. And what that spoke to was, in part, that working through covid was really taxing. Women were more often in positions that were on the front lines, but what it also spoke to is that the culture of medicine has long been very unfriendly toward the family-building burdens that often fall on women, and that hasn’t gotten better. If anything, it’s gotten worse because child care is even harder to come by. Moms, in particular, have way more to juggle and to balance than they once did. And the support, it’s not even fair to say it hasn’t caught up. It was never there to begin with.
Weber: And just to add on that, I mean, I find it — that study is great, and I will say I have family members that struggle with this currently. It’s wild to me that the American Academy of Pediatrics recommends a 12-week parental leave, and you possibly couldn’t finish your residency or qualify for a surgery residency if you take more than six weeks. I mean, I think that, in itself, that factoid really says exactly what Shefali was getting at. The culture of medicine is not at all friendly to folks that are considering this whatsoever.
Rovner: There’s so many women in medicine now. Now it’s making a problem not just for the women in medicine, but for everybody who wants medical care. So maybe that will get some attention paid to it. Moving on to “This Week in Private Equity,” we have another study from the Journal of the American Medical Association. It found that hospitals that were bought by private equity firms had a 25% increase in adverse events in the three years following their acquisition. Adverse events include things like falls, hospital-acquired infections, and other harm that, in theory, could or should have been prevented. It’s not really hard to connect the dots here, right? Private equity wants to raise more money, and that tends to want to cut staff, so bad things happen. I see you nodding, Victoria.
Knight: Yeah, I mean, I think this is an ongoing issue. It’s something that the Biden administration has said they want to look into, just decreasing quality of care in places that are taken over by private equity. I’m not sure there’s a really good solution to it at this point in time. And I think it also speaks to the broader issues of consolidation among the health care industry and the business of health care and what that means in regards to quality for patients. But yeah, I think this study is just another piece in building up a case of why sometimes private equity doesn’t always seem to equate to the best care for patients.
Luthra: If we go back in time a little bit, there is more evidence that shows the role that private equity has played in not only reduction in quality of care, but in the opposition between the health care industry and consumers. And the example I’m thinking of is air ambulances and surprise billing by those ER staffing firms, all of which were eventually owned by private equity firms that have their own set of incentives that is at odds with the goal of providing care that people can afford and can access, and that keeps them healthy.
Rovner: Indeed. Well, following “This Week in Private Equity,” we have “This Week in Health Misinformation.” My winner this week is Robert F. Kennedy Jr., who was awarded the “Lie of the Year” from PolitiFact for not just his repeated and repeatedly debunked claims about vaccines, but other fanciful conspiracy theories about covid-19, mass shootings, and the rise in gender dysphoria. I will post the link so I don’t have to repeat all of those things here. Which brings us to the story I asked Lauren here to talk about, how the anti-vax movement is quietly gaining a foothold in state houses. Lauren, tell us what you found.
Weber: Well, I found that it’s becoming very politically advantageous, to some extent. Political clout around anti-vaccine movement is growing. So you’re seeing more and more state legislators get elected that have anti-vaccine or vaccine-skeptical views. And I went down to Baton Rouge and 29 folks that were supported by Stanford Health Freedom, which is against vaccine mandates, got elected in this year’s off-cycle elections. So who knows what will happen next year, but you’re already seeing this reflected in other states. In Iowa, legislators this year stopped the requirement that you can talk about the HPV vaccines in schools. In Tennessee, home-schooled kids no longer have vaccine requirements. In Florida, they banned any possible requiring of covid vaccines, which experts said they worry if you just strike “covid” from that, that could lead to the banning of other requirements for vaccines. You’re seeing this momentum grow, and as you mentioned, Julie, RFK Jr. has played a role in this.
As I talk about in my story, back in 2021, he went down to Louisiana and really riled up some anti-vaccine fever in a legislative hearing about the covid vaccine. And so it’s a combination of things. People are reacting to a lot of misinformation that was spread during covid about the covid vaccine. And that distrust of the covid vaccine is seeping into childhood vaccinations. I mean, this year we saw data that came out that said in the 2022-2023 school year, we saw the highest rate of exemption rates for kindergartners getting their vaccinations. That’s a bad trend for the United States when it comes to herd immunity to protect against things like measles or other preventable diseases. So we will see how the next year plays out legislatively, but as it stands right now, I expect to see much more anti-vaccine movement in the statehouses in 2024.
Rovner: I’ve been covering the anti-vax movement for, I don’t know, 25, 30 years. There’s always been an anti-vax movement. It’s actually this combination of people on the far left and people on the far right, they tend to both be anti-vax, but I think this is the first time we’ve really seen it come into actual legislating way. In fact, the trend over the last couple of years has been to get rid of things like religious exemptions for families getting their children vaccinated in order to attend public school. So now we’re expecting to see the reverse, right?
Weber: Yeah, as you said, this is a horseshoe political issue that it’s been far left, far right, but now it’s really seeped into the far-right conservative consciousness in a way that has become a political advantage for some candidates. And so you’re seeing stuff that would previously be, not even make it to the floor for a vote, have to be vetoed, make it out of a committee, where previously some of these things would’ve looked at the signs and said, this is just not true. Now there’s more political power behind the ideology of some of these anti-mandate freedom pushes. So it’s really going to be something to track in this upcoming year.
Rovner: I think the other trend we’re seeing is actual health officials talking about these kinds of things, led by the Florida Surgeon General, Dr. [Joseph] Ladapo. He’s now moved on beyond recommending that young men not get the covid vaccine, right?
Weber: Yeah. So yesterday he sent out a health bulletin, and I just want to take a step back to say this is incredibly unprecedented because this is a state health officer sending out a bulletin to the state saying that he does not recommend anyone … he wants to halt the use of mRNA covid vaccinations. Now, that is not a position that any other state health officer has taken. It’s not a position that any national health agency has taken. He made it based on claims that have been debunked. He primarily based it on a study that several of the experts I talked to said it is not one that they would base assumptions on.
His claims were implausible, but needless to say, I mean, he’s the health director for the third-largest state in the union. I mean, his words carry weight, and his political patron is Ron DeSantis. Now, DeSantis has not commented publicly yet on this, but oftentimes it seems that they both have worked hand in hand to fight against vaccine mandates and to cause a ruckus around things like this. So it needs to be seen the politicization of this as this continues to play out.
Rovner: Well, that is a wonderful segue into our interview this week with Dr. Sandro Galea about the future of public health. So we will play that now and then we will come back and do our extra credits.
I am pleased to welcome to the podcast Dr. Sandro Galea, dean of the Boston University School of Public Health. Longtime listeners will know I’ve been concerned about the state of public health since even before the pandemic. Dr. Galea has a new book of essays called “Within Reason: A Liberal Public Health for an Illiberal Time” that takes a pretty provocative look at what’s gone wrong for public health and how it might win back the support of the actual public. Dr. Galea, thank you so much for joining us.
Sandro Galea: Thank you for having me.
Rovner: So I want to start with your diagnosis of what it is that ails public health in 2024.
Galea: Well, I suppose I start from the data, and the data show that there is a tremendous loss of trust in science broadly, in public health more specifically. Data from Pew that came out just a few months ago show, really, a 25-point drop in trust in medicine and in health from before the pandemic. So the question becomes why is that? What’s going on? And what I try to do in the book is to identify a number of things that I think have really hurt us, and I could numerate those. No. 1, it is we took a very narrow approach to our perception of what should have been done without leaving space for a plurality of voices that weigh different inputs differently.
No. 2, that through the mediation of social media as a way of extending our voice, we were perhaps inhabited false certitude much more than we ever meant to or much more than we do when we think about our science. And No. 3, we allowed ourselves to become politicized in a way that’s unhealthy. Perhaps partisanized is an even better term because public health is always political, but we allowed ourselves to become blue versus red, and that doesn’t serve anybody because public health should be there to serve the whole public. And I think those three big buckets, obviously in the book I write about them in much more detail, but I think they capture the fundamental problems that then have resulted in this loss of trust we face right now.
Rovner: So I’ve had experts note that the lack of public trust in public health isn’t necessarily because of anything the public health community has done. It’s because of a broader pushback against elites and people in power of all kinds. Do you think that’s the case, or has public health also contributed to its own, I won’t say downfall, but lack of status?
Galea: I feel like the answer to that is “and,” meaning that, yes, there’s no question that there are forces that have tried to undermine public health, forces that tried to undermine science. And in the book, I’m very clear that I do realize there are outside forces that have had mal intent, that they have not acted in good faith and they have tried to undermine public health and science, but that’s not what the book is about. I say that is there, I recognize it’s there, but I wanted to write about public health from within public health. It would be shortsighted of us not to realize that we are contributing to how public perceives us. In many respects, I feel like we should have the agency and the confidence to say, well, there are things that we are doing that we should look at. And now, after the acute phase of the pandemic, is the time to look at that.
I was clear in my other writing that I did not write this book in 2021 or 2022 intentionally, because it was too close. But I feel like now that we’re over the acute phase of the pandemic, now is the time to ask hard questions and to say, “What should we be learning?” And I do that in the book, very much looking forward. I’m not naming names, I’m not pointing fingers. All I’m simply saying is we now have the benefit of time passing. Let us see what we should have done better so we can learn how to be better in future.
Rovner: One of the things I think that frustrated me as a journalist, as somebody who communicates to a lay audience for a living, is that public health and science in general during the pandemic seemed unable to say that yes, as we learn more, we’re going to change what we recommend. It becomes, to the public, well, they said this and now they’re saying that, so they were wrong. Does public health need to show its work more?
Galea: This is the term that I use, which is false certitude, which is that we conveyed confidence when we should not have conveyed confidence. Now, there are many reasons for that. Things were happening quickly. It was a fast-moving pandemic. Everybody was scared. And, also, our communication was mediated through social media, which was a new medium for communication of public health. And that does not leave space for the asterisk, for the caveat. And I think our mistake was not recognizing how much harm it was going to do and not being upfront about this is what we know today, but tomorrow we may know more, and we may then have to change our recommendations. And as one pauses and thinks about how should we do better, surely this is front and center to learn how to communicate by saying, “Today, based on what we know, this is what we think is best, but we reserve the right to come back tomorrow and be clear, tell you that the data have changed, hence the recommendations have changed.”
Rovner: Do you think public health has been slow to embrace things like social media? I mean, there are organizations on social media. I think one that comes to mind is the Consumer Product Safety Commission, the National Park Service. I mean that they’re very cheeky, but they get out really important information in a very quick and understandable way. Is that something that public health needs to be doing better?
Galea: Perhaps. I’m not sure I’m willing to say that public health is any worse than the National Park Service on social media. I think we are all, as a society, struggling with communicating important facts rapidly in a time of crisis. One analogy, which I use in the book, is the analogy to 9/11, meaning in 9/11, it was the first national crisis that was lived through in a time of 24/7 cable news. And as a result, there was a lot of noise on cable news that was happening that was distorting how we dealt with the event. Similarly, covid-19 was the first national crisis that was lived through the lens of social media, and we did not really know how to use it. So, at the same time as I’m labeling this as a real challenge that public health faced, I’m also trying to understand and have the compassion to realize that in public health we were struggling to learn how to do this as everybody else was.
Rovner: So let’s turn to the future. What should public health do first to try and regain some of the trust that it’s lost?
Galea: Well, I suppose first we should be having this conversation, and I’m grateful to you for having a conversation, but I actually mean that, at a large scale, I actually think that I meant my book to be a place marker. And I say in it clearly, I expect people will disagree with elements of the book, and that’s OK. And I hope that the book encourages others to write their books that talks about the things, how they see it. Because I do think that this conversation should open up space for public health to say, what are the things that we didn’t do well? What are the things that we should do better? Because from that is going to emerge a new consensus about how we should act.
If the only thing that emerges is simply this, what you and I just talked about, which is communicating with due humility, recognizing the complexity of rapidly evolving facts, and being clear with the population that things may change. If that’s the only thing that emerges, we’ve already made progress. So I think the first thing that should happen is having the conversation, opening this up, being honest that there are things that public health did that it should do better. That is going to lead us to a new consensus about how we should do better.
Rovner: And beyond the conversation, is there one thing that you wish that policymakers could do that could help public health regain its prominence and its trust? I mean, there really is no other word here.
Galea: I think the one thing that I would want to see in policy is a moving away from abolishing of the notion that we can “follow the science.” One of my least favorite things that happened during the pandemic was this notion that we could “follow the science.” Now, why do I say that? I’m a scientist! But I say that because “follow the science” implies that science leads to linear answers, to linear solutions. And that phrase, “follow the science,” became a fig leaf for policymakers, saying, “Well, the science says we should do X, therefore we’re going to do X.” That is simply false. Policymaking should rest on multiple inputs, science being one of them, but also values, but also the importance of other sectors of the economy.
And I would like us to see as a society being honest about that, that policymaking shouldn’t take science into account centrally. I agree with that. As I said, it’s my bread and butter, it’s what I do. But to pretend that science has the answer is simply wrong. We elect people in elected positions, and there are people who are appointed in decision-making positions in other circumstances. It is their job to weigh all the inputs, science being one of those inputs.
Rovner: Well, Dr. Galea, thank you so much. I will do my part to keep the conversation going. I’m sure you will do yours as well.
Galea: I will. And thank you for doing the part you’re doing.
Rovner: OK. We are back and it’s time for our extra-credit segment. That’s when we each recommend a story we read this week we think you should read, too. As always, don’t worry if you miss it. We will post the links on the podcast page at kffhealthnews.org and in our show notes on your phone or other mobile device. Shefali, why don’t you go first this week?
Luthra: Sure. My story is from Stat by Nicholas Florko. The headline is “Medical Marijuana Companies Are Using Pharma’s Sales Tactics With Little of the Same Scrutiny.” And I think this is such a smart investigation, and I’m so grateful that Nicholas wrote it. It really gets into the fact that medical marijuana is a tremendous industry now, right? It’s not just in the Colorados or the Californias or Massachusetts that you think of. It’s all over the country and it’s a huge business. And because it’s so new, it hasn’t gotten the same scrutiny in terms of how it markets its products to consumers, the relationship it has with providers, et cetera. I think this is just a really important topic, and it’s something that we should all be paying attention to as the industry continues to grow in the coming years.
Rovner: Indeed. Victoria?
Knight: Yeah. So my extra credit this week is a Politico story by Megan Messerly and Robert King titled “Georgia Offered Medicaid With a Work Requirement. Few Have Signed Up.” And so it’s talking about just the rollout of Georgia implementing a work requirement for their Medicaid program, which they did expand Medicaid, but they included a work requirement. So I thought this was just really stunning. It said through the first four months, only 1,800 people have enrolled when the governor, Brian Kemp, expected 31,000 people to sign up.
Rovner: Contrast that with North Carolina, which expanded Medicaid without the work requirement and got, like, 200,000 people to sign up.
Knight: Yeah. So that’s just a stunning number. And they’re talking about in the story there. They’re not sure why all the reasons are, but part of it is that there is a lot of paperwork involved. And so I think it was just a really interesting example. Obviously, we have seen work requirements play out before, but we haven’t seen it in a while. And so it’s interesting to see how difficult it can be for people to access Medicaid if this is put in place. And I also think it’s important to remind people that last year, in 2023, during the debt ceiling debate, Republicans did for a while talk about wanting to implement work requirements in Medicaid again. And so, if this was something that they put into place, it would mean probably a lot of people would drop off the rolls. So it’s an idea that resurfaces. So just important to remember that.
Rovner: Indeed. Lauren.
Weber: I was obsessed with Greg Jaffe story from The Washington Post titled “Can the Exhausted, Angry People of Ottawa County Learn to Live Together?” And it’s this incredible portrait of this Michigan county where the county public health officer, Adeline Hambley, has come under tremendous pressure and threat from the conservative county board. And this is a story we have seen play out in different iterations all around the country in the wake of covid. It’s the “we don’t believe in masks, we don’t believe in shutdowns” versus the county public health folks who are trying to follow the science and how does that play out at a people level, which Greg just does a fantastic way of showing. And it’s interesting, the board was so fed up with her and making such political statements that they offered her $4 million to quit. Now this fell apart because the county doesn’t seem to have the money that would affect them, et cetera.
But it just goes to show how deep the divisions are between what used to be a very non-politicized, normal government job of being a public health officer who keeps your water safe and tries to keep you from catching bad diseases at restaurants, to the post-covid era, where [they’re] just absolutely vilified and hated, really, it seems in some of these comments in the story — so much so that they would be paid this much money to quit. So I think this speaks a lot to the tension that we see in America around public health today, and I really recommend everybody to give it a read.
Rovner: Yeah, it’s a really remarkable story. Well, my extra credit this week is from our podcast pal Alice [Miranda] Ollstein, along with her colleagues Jessica Piper and Madison Fernandez at Politico. It’s called Why Democrats Can’t Rely on Abortion Ballot Initiatives to Help Them Win.” And it’s a warning for Democrats not to get too smug about the popularity and success of abortion rights ballot measures around the country. They dug into the numbers and found that in many of those states, the very same voters who supported the abortion rights measures also turned around and voted for Republican candidates. As usual, in politics, things are rarely as simple as they seem.
All right, that is our show for this first week of 2024. As always, if you enjoy the podcast, you can subscribe wherever you get your podcasts. We’d appreciate it if you left us a review; that helps other people find us, too. Special thanks, as always, to our technical guru, Francis Ying, and our editor, my fellow Wolverine, Emmarie Huetteman. As always, you can email us your comments or questions. We’re at whatthehealth@kff.org, or you can still find me at X, @jrovner, or @julierovner at Bluesky and @julie.rovner at Threads. Shefali, where are you these days?
Luthra: I am @shefalil on X and Blue Sky, and then on Threads, I’m @shefali.luthra.
Rovner: Victoria.
Knight: I’m @victoriaregisk on X and Threads.
Luthra: Lauren.
Weber: And then I’m @LaurenWeberHP on X and clearly still need to work on my social media game.
Rovner: We will be back in your feed next week. Until then, be healthy.
Credits
Francis Ying
Audio producer
Emmarie Huetteman
Editor
To hear all our podcasts, click here.
And subscribe to KFF Health News’ “What the Health?” on Spotify, Apple Podcasts, Pocket Casts, or wherever you listen to podcasts.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
california, Courts, Multimedia, States, Abortion, Hospitals, KFF Health News' 'What The Health?', Misinformation, Podcasts, texas, U.S. Congress
‘Financial Ruin Is Baked Into the System’: Readers on the Costs of Long-Term Care
Thousands of readers reacted to the articles in the “Dying Broke” series about the financial burden of long-term care in the United States. They offered their assessments for the government and market failures that have drained the lifetime savings of so many American families. And some offered possible solutions.
Thousands of readers reacted to the articles in the “Dying Broke” series about the financial burden of long-term care in the United States. They offered their assessments for the government and market failures that have drained the lifetime savings of so many American families. And some offered possible solutions.
In more than 4,200 comments, readers shared their struggles in caring for spouses, older parents, and grandparents. They expressed anxieties about getting older themselves and needing help to stay at home or in institutions like nursing homes or assisted living facilities.
Many suggested changes to U.S. policy, like expanding the government’s payments for care and allowing more immigrants to stay in the country to help meet the demand for workers. Some even said they would rather end their lives than become a financial burden to their children.
Many readers blamed the predominantly for-profit nature of American medicine and the long-term care industry for depleting the financial resources of older people, leaving the federal-state Medicaid programs to take care of them once they were destitute.
“It is incorrect to say the money isn’t there to pay for elder care,” Jim Castrone, 72, a retired financial controller in Placitas, New Mexico, commented. “It’s there, in the form of profits that accrue to the owners of these facilities.”
“It is a system of wealth transference from the middle class and the poor to the owners of for-profit medical care, including hospitals and the long-term care facilities outlined in this article, underwritten by the government,” he added.
Other readers pointed to insurance policies that, despite limitations, had helped them pay for services. And some relayed their concerns that Americans were not saving enough and were unprepared to take care of themselves as they aged.
What Other Nations Provide
Other countries’ treatment of their older citizens was repeatedly mentioned. Readers contrasted the care they observed older people receiving in foreign countries with the treatment in the United States, which spends less on long-term care as a portion of its gross domestic product than do most wealthy nations.
Marsha Moyer, 75, a retired teaching assistant in Memphis, Tennessee, said she spent 12 years as a caregiver for her parents in San Diego County and an additional six for her husband. While they had advantages many don’t, Moyer said, “it was a long, lonely job, a sad job, an uphill climb.”
By contrast, her sister-in-law’s mother lived to 103 in a “fully funded, lovely elder care home” in Denmark during her last five years. “My sister-in-law didn’t have to choose between her own life, her career, and helping her healthy but very old mother,” Moyer said. “She could have both. I had to choose.”
Birgit Rosenberg, 58, a software developer in Southampton, Pennsylvania, said her mother had end-stage dementia and had been in a nursing home in Germany for more than two years. “The cost for her absolutely excellent care in a cheerful, clean facility is her pittance of Social Security, about $180 a month,” she said. “A friend recently had to put her mother into a nursing home here in the U.S. Twice, when visiting, she has found her mother on the floor in her room, where she had been for who knows how long.”
Brad and Carol Burns moved from Fort Worth, Texas, in 2019 to Chapala, Jalisco, in Mexico, dumping their $650-a-month long-term care policy because care is so much more affordable south of the border. Brad, 63, a retired pharmaceutical researcher, said his mother lived just a few miles away in a memory care facility that costs $2,050 a month, which she can afford with her Social Security payments and an annuity. She is receiving “amazing” care, he said.
“As a reminder, most people in Mexico cannot afford the care we find affordable and that makes me sad,” he said. “But their care for us is amazing, all health care, here, actually. At her home, they address her as Mom or Barbarita, little Barbara.”
Insurance Policies Debated
Many, many readers said they could relate to problems with long-term care insurance policies, and their soaring costs. Some who hold such policies said they provided comfort for a possible worst-case scenario while others castigated insurers for making it difficult to access benefits.
“They really make you work for the money, and you’d better have someone available who can call them and work on the endless and ever-changing paperwork,” said Janet Blanding, 62, a technical writer in Fancy Gap, Virginia.
Derek Sippel, 47, a registered nurse in Naples, Florida, cited the $11,000 monthly cost of his mother’s nursing home care for dementia as the reason he bought a policy. He pays about $195 a month with a lifetime benefit of $350,000. “I may never need to use the benefit[s], but it makes me feel better knowing that I have it if I need it,” he said in his comment. He said he could not make that kind of money by investing on his own.
“It’s the risk you take with any kind of insurance,” he said. “I don’t want to be a burden on anyone.”
Pleas for More Immigrant Workers
One solution that readers proposed was to increase the number of immigrants allowed into the country to help address the chronic shortage of long-term care workers. Larry Cretan, 73, a retired bank executive in Woodside, California, said that over time, his parents had six caretakers who were immigrants. “There is no magic bullet,” he said, “but one obvious step — hello, people — we need more immigrants! Who do you think does most of this work?”
Victoria Raab, 67, a retired copy editor in New York, said that many older Americans must use paid help because their grown children live far away. Her parents and some of their peers rely on immigrants from the Philippines and Eritrea, she said, “working loosely within the margins of labor regulations.”
“These exemplary populations should be able to fill caretaker roles transparently in exchange for citizenship because they are an obvious and invaluable asset to a difficult profession that lacks American workers of their skill and positive cultural attitudes toward the elderly,” Raab said.
Federal Fixes Sought
Other readers called for the federal government to create a comprehensive, national long-term care system, as some other countries have. In the United States, federal and state programs that finance long-term care are mainly available only to the very poor. For middle-class families, sustained subsidies for home care, for example, are fairly nonexistent.
“I am a geriatric nurse practitioner in New York and have seen this story time and time again,” Sarah Romanelli, 31, said. “My patients are shocked when we review the options and its costs. Medicaid can’t be the only option to pay for long-term care. Congress needs to act to establish a better system for middle-class Americans to finance long-term care.”
John Reeder, 76, a retired federal economist in Arlington, Virginia, called for a federal single-payer system “from birth to senior care in which we all pay and profit-making [is] removed.”
Other readers, however, argued that people needed to take more responsibility by preparing for the expense of old age.
Mark Dennen, 69, in West Harwich, Massachusetts, said people should save more rather than expect taxpayers to bail them out. “For too many, the answer is, ‘How can we hide assets and make the government pay?’ That is just another way of saying, ‘How can I make somebody else pay my bills?’” he said, adding, “We don’t need the latest phone/car/clothes, but we will need long-term care. Choices.”
Questioning the Value of Life-Prolonging Procedures
A number of readers condemned the country’s medical culture for pushing expensive surgeries and other procedures that do little to improve the quality of people’s few remaining years.
Thomas Thuene, 60, a consultant in Boston’s Roslindale neighborhood, described how a friend’s mother who had heart failure was repeatedly sent from the elder care facility where she lived to the hospital and back, via ambulance. “There was no arguing with the care facility,” he said. “However, the moment all her money was gone, the facility gently nudged my friend to think of end-of-life care for his mother. It seems the financial ruin is baked into the system.”
Joan Chambers, 69, an architectural draftsperson in Southold, New York, said that during a hospitalization on a cardiac unit she observed many fellow patients “bedridden with empty eyes,” awaiting implants of stents and pacemakers.
“I realized then and there that we are not patients, we are commodities,” she said. “Most of us will die from heart failure. It will take courage for a family member to refuse a ‘simple’ procedure that will keep a loved one’s heart beating for a few more years, but we have to stop this cruelty.
“We have to remember that even though we are grateful to our health care professionals, they are not our friends. They are our employees and we can say no.”
One physician, James Sullivan, 64, in Cataumet, a neighborhood of Bourne, Massachusetts, said he planned to refuse hospitalization and other extraordinary measures if he suffered from dementia. “We spend billions of dollars, and a lot of heartache, treating demented people for pneumonia, urinary tract infections, cancers, things that are going to kill them sooner or later, for no meaningful benefit,” Sullivan said. “I would not want my son to spend his good years, and money, helping to maintain me alive if I don’t even know what’s going on,” he said.
Considering ‘Assisted Dying’
Others went further, declaring they would rather arrange for their own deaths than suffer in greatly diminished capacity. “My long-term care plan is simple,” said Karen Clodfelter, 65, a library assistant in St. Louis. “When the money runs out, I will take myself out of the picture.” Clodfelter said she helped care for her mother until her death at 101. “I’ve seen extreme old age,” she said, “and I’m not interested in going there.”
Some suggested that medically assisted death should be a more widely available option in a country that takes such poor care of its elderly. Meridee Wendell, 76, of Sunnyvale, California, said: “If we can’t manage to provide assisted living to our fellow Americans, could we at least offer assisted dying? At least some of us would see it as a desirable solution.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
Aging, Health Care Costs, Health Industry, Aid In Dying, california, Dying Broke, Florida, Legislation, Long-Term Care, Massachusetts, Missouri, New Mexico, New York, Pennsylvania, Tennessee, texas, Virginia
As Foundation for ‘Excited Delirium’ Diagnosis Cracks, Fallout Spreads
When Angelo Quinto’s family learned that officials blamed his 2020 death on “excited delirium,” a term they had never heard before, they couldn’t believe it. To them, it was obvious the science behind the diagnosis wasn’t real.
Related Links
-
Police Blame Some Deaths on ‘Excited Delirium.’ ER Docs Consider Pulling the Plug on the Term.
Oct 2, 2023
-
California Bans Controversial ‘Excited Delirium’ Diagnosis
Oct 12, 2023
-
Doctors Abandon a Diagnosis Used to Justify Police Custody Deaths. It Might Live On, Anyway.
Oct 16, 2023
Quinto, 30, had been pinned on the ground for at least 90 seconds by police in California and stopped breathing. He died three days later.
Now his relatives are asking a federal judge to exclude any testimony about “excited delirium” in their wrongful death case against the city of Antioch. Their case may be stronger than ever.
Their push comes at the end of a pivotal year for the long-standing, nationwide effort to discard the use of excited delirium in official proceedings. Over the past 40 years, the discredited, racially biased theory has been used to explain away police culpability for many in-custody deaths. But in October, the American College of Emergency Physicians disavowed a key paper that seemingly gave it scientific legitimacy, and the College of American Pathologists said it should no longer be cited as a cause of death.
That same month, California’s Democratic Gov. Gavin Newsom signed the nation’s first law to ban the term “excited delirium” as a diagnosis and cause of death on death certificates, autopsy reports, and police reports. Legislators in other states are expected to consider similar bills next year, and some law enforcement agencies and training organizations have dropped references to excited delirium from their policy manuals and pulled back from training police on the debunked theory.
Despite all that momentum, families, attorneys, policing experts, and doctors say much remains to be done to correct the mistakes of the past, to ensure justice in ongoing trials, and to prevent avoidable deaths in the future. But after years of fighting, they’re heartened to see any movement at all.
“This entire thing, it’s a nightmare,” said Bella Collins, Angelo’s sister. “But there are silver linings everywhere, and I feel so fortunate to be able to see change happening.”
Ultimately, the campaign against excited delirium seeks to transform the way police deal with people undergoing mental health crises.
“This is really about saving lives,” said Joanna Naples-Mitchell, an attorney who worked on an influential Physicians for Human Rights review of excited delirium.
Changing Law Enforcement Training
The use of the term “excited delirium syndrome” became pervasive after the American College of Emergency Physicians published a white paper on it in 2009. It proposed that individuals in a mental health crisis, often under the influence of drugs or alcohol, can exhibit superhuman strength as police try to control them, and then die suddenly from the condition, not the police response.
The ACEP white paper was significant in catalyzing police training and policy, said Marc Krupanski, director of criminal justice and policing at Arnold Ventures, one of the largest nonprofit funders of criminal justice policy. The theory contributed to deaths, he said, because it encouraged officers to apply greater force rather than call medical professionals when they saw people in aggressive states.
After George Floyd’s 2020 death, which officers blamed on excited delirium, the American Medical Association and the American Psychiatric Association formally rejected it as a medical condition. Then came disavowals from the National Association of Medical Examiners and the emergency physicians’ and pathologists’ groups this year.
The moves by medical societies to renounce the term have already had tangible, albeit limited, effects. In November, Lexipol, a training organization used by thousands of public safety agencies in the U.S., reiterated its earlier move away from excited delirium, citing the California law and ACEP’s retraction of the 2009 white paper.
Lexipol now guides officers to rely on what they can observe, and not to guess at a person’s mental status or medical condition, said Mike Ranalli, a lawyer and police trainer with the Texas-based group. “If somebody appears to be in distress, just get the EMS,” he said, referring to emergency medical services.
Patrick Caceres, a senior investigator at the Bay Area Rapid Transit’s Office of the Independent Police Auditor, successfully pushed to remove excited delirium from the BART Police Department’s policy manual after learning about Quinto’s death in 2020 and seeing the American Medical Association’s rejection of it the following year.
Caceres fears that rooting out the concept — not just the term — more broadly will take time in a country where law enforcement is spread across roughly 18,000 agencies governed by independent police chiefs or sheriffs.
“The kinds of training and the kinds of conversations that need to happen, we’re still a long way away from that,” said Caceres.
In Tacoma, Washington, where three police officers have been charged with the 2020 death of Manuel Ellis, The Seattle Times reported that local first responders testified as recently as October that they still “embrace” the concept.
But in Colorado, the state’s Peace Officer Standards and Training board ruled on Dec. 1 to drop excited delirium training for new law enforcement officers, KUSA-TV reported.
And two Colorado lawmakers, Democratic state Reps. Judy Amabile and Leslie Herod, have drafted a bill for the 2024 legislative session banning excited delirium from other police and EMS training and prohibiting coroners from citing it as a cause of death.
“This idea that it gives you superhuman strength causes the police to think they should respond in a way that is often completely inappropriate for what’s actually happening,” Amabile said. “It just seems obvious that we should stop doing that.”
She would like police to focus more on de-escalation tactics, and make sure 911 calls for people in mental health crisis are routed to behavioral health professionals who are part of crisis intervention teams.
Taking ‘Excited Delirium’ Out of the Equation
As the Quinto family seeks justice in the death of the 30-year-old Navy veteran, they are hopeful the new refutations of excited delirium will bolster their wrongful death lawsuit against the city of Antioch. On the other side, defense lawyers have argued that jurors should hear testimony about the theory.
On Oct. 26, the family cited both the new California law and the ACEP rebuke of the diagnosis when it asked a U.S. District Court judge in California to exclude witness testimony and evidence related to excited delirium, saying it “cannot be accepted as a scientifically valid diagnosis having anything to do with Quinto’s death.”
“A defense based on BS can succeed,” family attorney Ben Nisenbaum said. “It can succeed by giving jurors an excuse to give the cops a way out of this.”
Meanwhile, advocates are calling for a reexamination of autopsies of those who died in law enforcement custody, and families are fighting to change death certificates that blame excited delirium.
The Maryland attorney general’s office is conducting an audit of autopsies under the tenure of former chief medical examiner David Fowler, who has attributed various deaths to excited delirium. But that’s just one state reviewing a subset of its in-custody deaths.
The family of Alexander Rios, 28, reached a $4 million settlement with Richland County, Ohio, in 2021 after jail officers piled on Rios and shocked him until he turned blue and limp in September 2019. During a criminal trial against one of the officers that ended in a mistrial this November, the pathologist who helped conduct Rios’ autopsy testified that her supervisor pressured her to list “excited delirium” as the cause of death even though she didn’t agree. Still, excited delirium remains his official cause of death.
The county refused to update the record, so his relatives are suing to force a change to his official cause of death. A trial is set for May.
Changing the death certificate will be a form of justice, but it won’t undo the damage his death has caused, said Don Mould, Rios’ stepfather, who is now helping to raise one of Rios’ three children.
“Here is a kid that’s life is upside down,” he said. “No one should go to jail and walk in and not be able to walk out.”
In some cases, death certificates may be hard to refile. Quinto’s family has asked a state judge to throw out the coroner’s findings about his 2020 death. But the California law, which takes effect in January and bans excited delirium on death certificates, cannot be applied retroactively, said Contra Costa County Counsel Thomas Geiger in a court filing.
And, despite the 2023 disavowals by the main medical examiners’ and pathologists’ groups, excited delirium — or a similar explanation — could still show up on future autopsy reports outside California. No single group has authority over the thousands of individual medical examiners and coroners, some of whom work closely with law enforcement officials. The system for determining a cause of death is deeply disjointed and chronically underfunded.
“One of the unfortunate things, at least within forensic pathology, is that many things are very piecemeal,” said Anna Tart, a member of the Forensic Pathology Committee of the College of American Pathologists. She said that CAP plans to educate members through conferences and webinars but won’t discipline members who continue to use the term.
Justin Feldman, principal research scientist with the Center for Policing Equity, said that medical examiners need even more pressure and oversight to ensure that they don’t find other ways to attribute deaths caused by police restraint to something else.
Only a minority of deaths in police custody now cite excited delirium, he said. Instead, many deaths are being blamed on stimulants, even though fatal cocaine or methamphetamine overdoses are rare in the absence of opioids.
Yet advocates are hopeful that this year marks enough of a turning point that alternative terms will have less traction.
The California law and ACEP decision take “a huge piece of junk science out of the equation,” said Julia Sherwin, a California civil rights attorney who co-authored the Physicians for Human Rights report.
Sherwin is representing the family of Mario Gonzalez, who died in police custody in 2021, in a lawsuit against the city of Alameda, California. Excited delirium doesn’t appear on Gonzalez’s death certificate, but medical experts testifying for the officers who restrained him cited the theory in depositions.
She said she plans to file a motion excluding the testimony about excited delirium in that upcoming case and similar motions in all the restraint-asphyxia cases she handles.
“And, in every case, lawyers around the country should be doing that,” Sherwin said.
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
california, Mental Health, States, Colorado, Emergency Medicine, Legislation, Maryland, Ohio, Washington
El condado de Los Angeles ofrece terapia virtual gratuita de salud mental para estudiantes
LOS ANGELES – Las escuelas públicas del condado de Los Angeles han puesto en marcha una ambiciosa iniciativa para ofrecer servicios gratuitos de salud mental a sus 1,3 millones de estudiantes de primaria y secundaria (K-12), una prueba clave del amplio programa de $4,700 millones del gobernador de California, Gavin Newsom, para hacer frente a la crisis de salud mental entre los jóvenes.
Impulsado por los planes Medi-Cal del condado —que proporcionan seguro médico a los residentes con bajos ingresos— en colaboración con su Oficina de Educación y el Departamento de Salud Mental, el programa se basa en servicios de teleterapia proporcionados por Hazel Health, una de las empresas que han surgido para hacer frente a la escasez nacional de servicios de salud mental, algo que se agravó durante la pandemia de covid-19.
La teleterapia es uno de los cuatro proyectos del condado de Los Angeles que recibirán en conjunto hasta $83 millones del Programa de Incentivos de Salud Mental para Estudiantes del estado, uno de los componentes del “plan maestro” del gobernador demócrata para subsanar las deficiencias en el acceso de los jóvenes a los servicios de salud mental.
El contrato de Hazel Health en Los Angeles tiene como meta ayudar a las escuelas sobrecargadas a hacer frente al aumento de la demanda de estos servicios. Promete ser una iniciativa piloto para demostrar tanto la eficacia de la terapia virtual para los alumnos, como la capacidad de educadores y administradores para gestionar eficazmente un programa extenso y delicado en colaboración con una empresa con fines de lucro.
Para algunos educadores y familias los resultados iniciales son prometedores.
Anjelah Salazar, de 10 años, dijo que el especialista de Hazel la ha ayudado a sentirse mucho mejor. La estudiante de quinto grado empezó a sufrir ataques de pánico diarios al cambiar de escuela este año a la primaria Stanton de Glendora.
Su madre, Rosanna Chavira, contó que no sabía qué hacer —aunque es coordinadora clínica de una empresa que trata enfermedades mentales— y le preocupaba no poder pagar un terapeuta que aceptara su seguro. Cuando Chavira supo de Hazel, no lo dudó.
“El hecho de que sea gratis y de que un profesional le enseñe estrategias para sobrellevar distintas situaciones significa mucho”, dijo Chavira. “Ya se notan los resultados”.
Salazar dijo que hasta ahora tuvo cinco citas virtuales con su terapeuta. Una técnica de afrontamiento que aprecia especialmente es un ejercicio de tapping: todas las noches, antes de acostarse, se presiona con el dedo un poquito los ojos, las mejillas, el pecho y las rodillas. Con cada toque, dice: “Soy valiente”.
Christine Crone, madre de Brady, alumno de séptimo grado, afirmó que aún no ha comprobado si las sesiones son eficaces para su hijo, que estudia en Arroyo Seco Junior High en Santa Clarita, pero sí sabe que las disfruta.
“Normalmente le cuesta llegar a tiempo y estar preparado, pero con estas sesiones siempre deja lo que está haciendo y es puntual”, dijo Crone. “Dice que su terapeuta es agradable, divertido y que es fácil hablar con él”.
Jennifer Moya, consejera de salud mental en la escuela primaria Martha Baldwin de Alhambra, una ciudad al este de Los Angeles, dijo que a sus alumnos les gusta la flexibilidad de la teleterapia, que les permite reunirse con los terapeutas en cualquier momento entre las 7 de la mañana y las 7 de la tarde.
“Esta generación de niños ha crecido en la era digital”, señaló Moya, que se encarga de remitir a los alumnos a Hazel en su centro. “Les encanta que esto sea fácil”.
Pablo Isais, consejero de salud mental en la escuela primaria Granada’s Alhambra, dijo que los servicios también pueden ser una solución provisional mientras un estudiante espera una cita en persona, que puede tomar de seis a ocho semanas.
“Ser capaz de comunicarles que hay servicios disponibles a los que pueden acceder en la próxima semana es increíble”, dijo Moya.
Hasta ahora, sólo 607 estudiantes del condado de Los Angeles han participado en las sesiones desde que se ofrecieron por primera vez, en Compton, en diciembre de 2022, explicó Alicia Garoupa, jefa de servicios de bienestar y apoyo de la Oficina de Educación. Ella reconoció algunos problemas iniciales, pero aseguró que Hazel es “otra herramienta en nuestra caja de herramientas”.
El estado confía en las empresas con fines de lucro
La teleterapia desempeña un papel cada vez más importante en las escuelas del país, a medida que educadores y trabajadores sociales se enfrentan a la presión de abordar los crecientes problemas de salud mental. Según un informe de abril de Chalkbeat, 13 de los 20 distritos escolares más grandes del país, incluido Los Angeles Unified, la han incorporado desde que comenzó la pandemia.
El acuerdo del condado de Los Angeles con Hazel prevé el pago a la empresa de hasta $20 millones hasta finales de 2024. Además, Hazel puede facturar a los seguros de los estudiantes.
La empresa con sede en San Francisco, fundada en 2015, ha recaudado $112,5 millones de inversores y tiene contratos en 15 estados. Entre las empresas que buscan los dólares destinados para la salud mental de los jóvenes están otra startup de San Francisco, Daybreak Health, graduada de la prestigiosa incubadora tecnológica Y Combinator, junto con BeMe, Brightline y Kooth.
California eligió a Brightline y Kooth para una iniciativa estatal de $532 millones, en 2024, sobre servicios virtuales de comportamiento juvenil, otro componente importante del plan maestro de Newsom. Algunos programas estatales y locales se superponen, reconoció Naomi Allen, cofundadora y CEO de Brightline, pero dijo que la oferta de Brightline es más amplia que lo que Hazel hace en las escuelas, con servicios que incluyen desde sesiones de coaching para cuidadores hasta recursos de meditación.
“El estado financia el acceso gratuito a los servicios para todos los niños del estado, lo cual es un programa extraordinariamente ambicioso”, afirmó Allen.
Aún así, quedan muchos interrogantes sobre la eficacia de la teleterapia para estudiantes. Tampoco ha resultado ser una fuente de ingresos segura para las empresas: Brightline despidió al 20% de su plantilla la primavera pasada, la segunda ronda de despidos en seis meses.
Complemento, no solución
Chelsy Duffer-Dunbar, que en aquel momento trabajaba para Los Angeles Unified como trabajadora social psiquiátrica, declaró a KFF Health News en octubre que aún no había trabajado con Hazel, pero señaló que el condado exige que un miembro del personal permanezca a la vista del estudiante durante sus citas y le ayude si surgen problemas técnicos.
“Le sigue quitando tiempo al personal”, aseguró Duffer-Dunbar. “Mi día ya es muy estresante. No puedo imaginar tener una evaluación por amenaza y otra por suicidio en el trabajo y luego tener que buscar a alguien para que se siente en esta sesión de terapia con el niño o la niña y su iPad”.
Duffer-Dunbar añadió que quiere que el distrito dé prioridad a los terapeutas en persona que trabajan con la comunidad local, especialmente para los niños más pequeños que tienen problemas con la teleterapia.
Duffer-Dunbar ha dejado el distrito por recortes presupuestarios que la obligaban a desempeñar un trabajo más agobiante.
Hazel insistió en que la teleterapia no es una solución para todas las situaciones.
“Es una oportunidad para ampliar el acceso”, apuntó Andrew Post, jefe de innovación de la empresa.
Colaboración entre educación y salud
Fue necesaria una complicada colaboración entre los distritos escolares, las agencias del condado y los dos planes de Medi-Cal, L.A. Care Health Plan y Health Net, para poner en marcha el programa de terapia escolar. Las normas de financiación estatales se diseñaron para ayudar a las entidades a trabajar juntas.
“Este programa nos ha ayudado a acercarnos a los distritos escolares”, comentó Michael Brodsky, director de salud comunitaria de L.A. Care Health Plan. “Si podemos tratar a los niños cuando van a la escuela y derivarlos para que reciban tratamiento mientras están en la escuela, eso es bueno”.
Hazel ofrece principalmente sesiones de terapia individual de corta duración con trabajadores sociales clínicos u otros consejeros, el 40% de los cuales son bilingües. Son los más indicados para prestar apoyo temporal a quienes tienen necesidades leves o moderadas, como los estudiantes que luchan contra el estrés académico o empiezan en una escuela nueva, pero también pueden derivar a pacientes para que reciban atención a largo plazo.
El mayor distrito inscrito en el programa, Los Angeles Unified, cuenta con el 41% de los alumnos del condado, pero no todos los distritos están preparados para dar el salto. Cuatro de cada 10 distritos han optado por no ofrecer los servicios de Hazel, lo que Garoupa atribuye en parte a la preocupación por el intercambio de información sobre los estudiantes.
El contrato con Hazel termina en diciembre de 2024, pero Garoupa dijo que la Oficina de Educación y sus socios tienen la intención de mantener los servicios hasta junio de 2025. Cualquier prórroga posterior dependerá de los resultados.
Sonya Smith, colega de Garoupa, indicó que la Oficina de Educación evaluará la eficacia de Hazel a través de una encuesta anual, informes mensuales de impacto y reuniones semanales.
“El número de estudiantes que utilizan Hazel va a ser, obviamente, una medida clave”, añadió Smith. “La tasa de utilización de Hazel es del 3% al 8%. Evaluaremos si esas cifras se mantienen, si los estudiantes acceden a la atención en el momento oportuno y si alivia la carga del personal escolar y los proveedores comunitarios”.
Esta historia fue producida por KFF Health News, que publica California Healthline, un servicio editorialmente independiente de la California Health Care Foundation.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
california, Mental Health, Noticias En Español, States, Children's Health, Latinos, Telemedicine
LA County Invests Big in Free Virtual Mental Health Therapy for K-12 Students
LOS ANGELES — Los Angeles County public schools are rolling out an ambitious effort to offer free mental health services to their 1.3 million K-12 students, a key test of California Gov. Gavin Newsom’s sweeping, $4.7 billion program to address a youth mental health crisis.
Spearheaded by the county’s Medi-Cal plans — which provide health insurance to low-income residents — in collaboration with its Office of Education and Department of Mental Health, the LA school program relies on teletherapy services provided by Hazel Health, one of a clutch of companies that have sprung up to address a nationwide shortage of mental health services that grew much worse during the covid-19 pandemic.
The teletherapy effort is one of four LA County projects that will collectively receive up to $83 million from the state’s Student Behavioral Health Incentive Program, one component of the Democratic governor’s “master plan” to address gaps in youth mental health care access.
LA’s Hazel Health contract is aimed at helping overburdened schools cope with a surge in demand for mental health services. It promises to be a telling case study in both the efficacy of virtual therapy for students and the ability of educators and administrators to effectively manage a sprawling and sensitive program in partnership with a for-profit company.
For some Los Angeles County educators and families, the initial results are promising.
Anjelah Salazar, 10, said her Hazel clinician has helped her feel a lot better. After the fifth grader switched to a new school this year, Stanton Elementary in Glendora, she started having panic attacks every day.
Her mom, Rosanna Chavira, said she didn’t know what to do — even though she’s a clinical coordinator for a company that treats mental health conditions — and worried she wouldn’t be able to find an affordable therapist who accepted their insurance. Once Chavira learned about Hazel, she jumped at the opportunity.
“This being free and having a licensed professional teaching her coping skills, it just means the world,” Chavira said. “You can already see changes.”
Salazar said she’s met with her virtual therapist five times so far. One coping technique that she especially appreciates is a tapping exercise: Every night before bed, she taps her eyes, her cheeks, her chest, and her knees. With each tap, she recites the same affirmation: “I am brave.”
Christine Crone, parent of seventh grader Brady, said she has yet to see if the sessions have been effective for her son, who attends Arroyo Seco Junior High in Santa Clarita, but she knows he enjoys them.
“He struggles normally with being on time and prepared, but with these sessions, he always stops what he is doing and makes sure he is logged in on time,” Crone said. “He says that his therapist is nice, fun, and easy to talk to.”
Jennifer Moya, a mental health counselor at Martha Baldwin Elementary in Alhambra, a city east of Los Angeles, said her students like the flexibility of teletherapy, which allows them to meet with clinicians anytime between 7 a.m. and 7 p.m.
“This generation of kids has grown up digital,” said Moya, who is in charge of referring students to Hazel at her school. “They love that this is easy.”
Pablo Isais, a mental health counselor at Alhambra’s Granada Elementary School, said the services can also be a stopgap while a student waits for an in-person appointment, which can take six to eight weeks.
“To be able to let them know that there are services available that they can access within the next week is amazing,” Moya said.
Thus far, early in the rollout, only 607 Los Angeles County students have participated in Hazel sessions since they were first offered, in Compton, in December 2022, said Alicia Garoupa, chief of well-being and support services for the Office of Education. She acknowledged some bumps in the rollout but said Hazel is “another tool in our toolbox.”
State Relies on For-Profit Ventures
Teletherapy is playing an increasingly important role in schools across the nation as educators and social workers face pressure to address growing mental health issues. According to an April Chalkbeat report, 13 of the nation’s 20 largest school districts, including Los Angeles Unified, have added teletherapy since the pandemic began.
LA County’s deal with Hazel calls for the company to be paid up to $20 million through the end of 2024. In addition, Hazel can bill students’ insurance.
The San Francisco-based company, founded in 2015, has raised $112.5 million from investors and has contracts in 15 different states. Other companies chasing youth mental health dollars include another San Francisco startup, Daybreak Health, a graduate of the prestigious Y Combinator tech incubator, along with BeMe, Brightline, and Kooth.
California chose Brightline and Kooth for a 2024 $532 million statewide initiative on virtual youth behavioral services, another important component of Newsom’s master plan. There is some overlap between the state and local programs, Brightline co-founder and CEO Naomi Allen acknowledged, but she said the Brightline offering is broader than what Hazel is doing in schools, with services including everything from coaching sessions for caregivers to meditation resources.
“The state is funding free access to services for every child in the state, which is just a remarkably ambitious program,” said Allen.
Still, many questions remain about the efficacy of teletherapy for students. It’s also proving to be no surefire moneymaker for the companies thus far: Brightline laid off 20% of its staff last spring, the second round of layoffs in six months.
Supplement, Not Solution
Chelsy Duffer-Dunbar, who at the time worked for Los Angeles Unified as a psychiatric social worker, told KFF Health News in October that she hadn’t yet worked with Hazel, but noted that the county requires that a member of staff stay within eyesight of the student during their appointments and assist if tech issues arise.
“It is still taking up staff time,” Duffer-Dunbar said. “My day is already so stressful. I can’t imagine having a threat assessment and a suicide assessment at work and then trying to scramble around to find someone to sit in on this therapy session with the kiddo and their iPad.”
Duffer-Dunbar said she wants the district to prioritize in-person clinicians who are immersed in the local community, especially for younger kids who have trouble engaging with teletherapy.
Duffer-Dunbar has since left the district in response to budget cuts that forced her into a more burdensome role.
Hazel emphasized that teletherapy is not a one-size-fits-all solution.
“It’s an opportunity to expand access,” said Andrew Post, chief of innovation at the company.
Education and Health Care Working Together
It took a complicated collaboration between school districts, county agencies, and the two Medi-Cal plans, L.A. Care Health Plan and Health Net, to set up the school therapy program. The state funding rules were designed to push the entities to work together.
“This program has helped us get closer to school districts,” said Michael Brodsky, senior medical director for community health at L.A. Care Health Plan. “If we can catch kids while they’re at school and refer them to get treatment while they’re in school, that’s good.”
Hazel provides primarily short-term one-to-one therapy sessions with clinical social workers or other licensed counselors, 40% of whom are bilingual. They are best suited to provide temporary support to those with mild to moderate needs, such as students struggling with academic stress or starting at a new school, but they can also make referrals for long-term care.
The largest district enrolled in the program, Los Angeles Unified, accounts for 41% of the county’s students, but not all districts are ready to take the leap. Four in 10 districts have opted to not offer Hazel’s services, which Garoupa attributes partially to data-sharing concerns.
The contract with Hazel ends in December 2024, but Garoupa said the Office of Education and its partners intend to maintain services through June 2025. Any extension beyond that will depend on the results.
Sonya Smith, a colleague of Garoupa’s, said the Office of Education will be continuously evaluating Hazel’s effectiveness through an annual survey, monthly impact reports, and weekly meetings.
“The number of students that are using Hazel is obviously going to be a key metric,” Smith said. “Hazel’s historic utilization rate is 3% to 8%. We’ll be evaluating if those numbers hold up, if students are accessing care in a timely manner, and if it’s lightening the burden for school staff and community-based providers.”
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
california, Mental Health, States, Children's Health, Latinos, Telemedicine
Encuesta revela que persiste la discriminación racial en la atención médica
Muchas personas de grupos raciales y étnicos minoritarios dicen que se preparan mentalmente para recibir insultos y ser prejuzgados antes de las citas médicas, según una nueva encuesta entre pacientes que reafirma la prevalencia de la discriminación racial en el sistema de salud de Estados Unidos.
La encuesta de KFF, que se realizó con casi 6,300 pacientes que han estado recibiendo atención en los últimos tres años, encontró que alrededor del 55% de los adultos de raza negra sienten que deben tener mucho cuidado con su apariencia para ser tratados de manera justa por los médicos y otros proveedores de atención de salud.
Casi la mitad de los pacientes hispanos, los Indio americanos y los nativos de Alaska sienten lo mismo, al igual que aproximadamente 4 de cada 10 pacientes asiáticos.
En comparación, el 29% de los blancos no hispanos encuestados dijeron que se preocupaban por su apariencia antes de las citas.
“En 2023, la noción de que cualquier persona debe prepararse para sufrir discriminación es triste por un lado y enojoso por el otro”, dijo Burgess Harrison, director ejecutivo de la National Minority Health Association, en un correo electrónico . “El estrés que causa, además de cualquier problema de salud involucrado… es una locura”.
La discriminación ha sido durante mucho tiempo una preocupación tanto para los pacientes como para los proveedores de atención médica, en un país en donde las disparidades raciales en los resultados de salud son enormes y particularmente desfavorables para las personas negras.
Un hombre hispano de 30 años de Illinois, que respondió a la encuesta de KFF, dijo a los investigadores que cuando va a sus citas médicas usa ropa con el logo de la universidad en donde trabaja. Se dio cuenta que cuando los proveedores se enteran que es profesor, lo escuchan más atentamente y lo involucran más en las decisiones médicas, dijo.
Una mujer asiática de 44 años de California dijo que sus médicos varones, blancos no hispanos, ignoraron sus preocupaciones sobre sus problemas respiratorios y le dijeron que “probablemente estaba pensando demasiado en respirar”. Más tarde le diagnosticaron asma.
Los dos encuestados no fueron identificados con nombre y apellido en el estudio.
La encuesta ofrece “una manera de cuantificar realmente cuáles son esas experiencias con el racismo y la discriminación, y las múltiples formas en las que luego impactan en la vida de las personas”, dijo Samantha Artiga, directora del programa de políticas de salud y equidad racial de KFF.
“Para las personas que han estado siguiendo estos temas durante mucho tiempo, los hallazgos no son inesperados”, agregó. Otros hallazgos del sondeo fueron:
- Un tercio de los adultos informaron al menos una de varias experiencias negativas con un proveedor de atención médica en los últimos tres años, como que un profesional asumiera algo sobre ellos sin preguntar, o sugiriera que ellos eran los responsables de su problema de salud.
- Casi una cuarta parte de los adultos negros, el 19% de los adultos nativos de Alaska y nativos americanos, el 15% de los adultos hispanos y el 11% de los adultos asiáticos dijeron que creían que habían sufrido un trato negativo debido a su raza u origen étnico.
- El 22% de las embarazadas o que dieron a luz en los últimos 10 años, de raza negra, dijeron que les negaron los analgésicos que pensaban necesitaban. Sólo el 10% de los adultos blancos no hispanos en circunstancias similares informaron la misma queja.
Cuando las personas no se sienten respetadas o bienvenidas por sus proveedores de salud, es posible que eso los desanime a buscar ayuda médica o que cambien de proveedor con más frecuencia, dijo Artiga. Los pacientes de poblaciones minoritarias “experimentan peor salud como resultado de un trato injusto en el sistema de atención médica”, agregó.
La encuesta también encontró que la discriminación fuera del sistema de atención médica tenía consecuencias para la salud. Las personas que dijeron haber experimentado discriminación en su vida cotidiana informaron dos veces más seguido que a menudo se sentían ansiosas, solas o deprimidas en comparación con aquellas que rara vez o nunca habían enfrentado discriminación.
La encuesta encontró que las personas negras que reportaron tonos de piel más oscuros tenían más probabilidades de haber sufrido discriminación que aquellos con piel más clara. También reveló “cómo persisten y prevalecen las experiencias de racismo y discriminación hoy en día, en la vida diaria y también en la atención médica, a pesar del aumento de las alertas y el abordaje sobre el racismo”, dijo Liz Hamel, directora de investigación de encuestas y opinión pública de KFF.
La diversidad entre los proveedores de atención médica es importante, según la encuesta. La mayoría de las personas de minorías que participaron en la encuesta dijeron que menos de la mitad de sus visitas médicas en los últimos tres años fueron con un proveedor de su misma raza u origen étnico. Los que sí vieron a un médico de su misma raza o etnia tuvieron más probabilidades de informar mejores experiencias, como que su médico les explicara las cosas “de una manera que pudieran entender” o les preguntara sobre otros factores de salud como su empleo, vivienda y acceso a alimentos y transporte.
El 40% de los adultos negros que vieron a proveedores de su mi raza reportaron haber discutido temas sociales y económicos, mientras que solo el 24% dijo haber charlado sobre estos temas con proveedores de otras razas.
Harrison, de la National Minority Health Association, escribió que “es vital un énfasis renovado en reclutar más personas de color en el campo de la atención médica”.
Agregó que la encuesta “ilustra dolorosamente que el prejuicio racial en la atención sanitaria es tan dañino como cualquier enfermedad”.
La “Encuesta sobre racismo, discriminación y salud” de KFF se realizó del 6 de junio al 14 de agosto en línea y por teléfono entre una muestra representativa a nivel nacional de adultos estadounidenses en inglés, español, chino, coreano y vietnamita.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
Health Industry, Noticias En Español, Race and Health, california, Disparities, Illinois, KFF, Latinos, Polls
California woman with painful fat deposit disorder gets ‘life-changing’ surgery, has ‘newfound freedom’
An estimated one in nine adult women struggle with an abnormal and painful fat buildup in the lower body — and no amount of diet or exercise can help.
An estimated one in nine adult women struggle with an abnormal and painful fat buildup in the lower body — and no amount of diet or exercise can help.
Lipedema, a relatively common but often overlooked disease, causes fat to accumulate in the lower part of the body, primarily the butt, thighs and calves.
For many women, like Molly Friar, an event planner in Sacramento, California, it can cause debilitating pain and impaired mobility.
In an effort to raise awareness of this condition, Friar, 53, spoke with Fox News Digital about her long journey to diagnosis — and what she calls her newfound "freedom."
HIDDEN BELLY FAT COULD SIGNAL ALZHEIMER’S DISEASE RISK 15 YEARS BEFORE SYMPTOMS SHOW UP, STUDY FINDS
Friar was just 11 years old when she started to notice that her body was different than everyone else’s, she said during a phone interview.
"The lipedema itself is governed by hormone changes, so that's when things really took off for me," she said. "My legs were different from every other girl in my class, and I started to get a bit of a stomach in my lower abdomen."
It was puzzling for Friar, who was very fit and athletic.
She played soccer, basketball and softball, and was also a cheerleader — yet no matter how active she was or how carefully she ate, her lower body carried an abnormal amount of fat.
"Somehow my legs and stomach were always disproportionately bigger than everybody else's," she said.
Adding complexity to the situation, Friar is adopted — so she had no context that might have predicted this genetic condition.
"I don't have pictures of my family to look at, to see a grandmother or an aunt or other women in my life that were affected by it," she said.
Friar felt "completely out of place," she said, as everyone else in her family was "super skinny" and she was not.
Friar was just 12 years old when her parents put her on a Weight Watchers program.
"They felt like that was the best thing they could do to help me," she said.
Throughout her adolescence and young adulthood, Friar worked out every day, biking to the gym and taking aerobics with all the adults.
"That’s absolutely where I started a battle of shame around my body — something I couldn't control," she said.
"I would eat less or not eat, and exercise more, and do all the things I could think of to outpace something that I didn't know existed."
She added, "I always felt like there was a person inside of me who was thin and just wanted to get out."
In addition to the body image struggles, Friar’s condition also came with extreme pain.
Lipedema causes inflammation and extreme bruising — "I would just brush up against something and get a bruise," said Friar.
The activities that were pleasant for other people, like getting a massage during a pedicure, created "excruciating pain" for Friar.
For someone with lipedema, she explained, running a hand over the skin is like touching a rocky beach — "you can feel the nodules like pebbles under the skin."
Other common symptoms include swelling, a feeling of heaviness in the legs and excess fatigue.
For some patients, the condition can cause difficulty walking, heightened anxiety and depression, joint issues, venous (vein) disease and other complications, according to Cleveland Clinic.
In 2016, when Friar was 45 years old, she lost 50 pounds — but didn’t lose a centimeter in her calves.
She started digging in to figure out what was going on. "I knew something wasn’t right," she said.
In her online research, it wasn’t long before Friar was looking at photos of women with lipedema, with abnormal fat deposits in their lower bodies.
"In that moment, I cried — it was like looking in a mirror," she told Fox News Digital.
"I felt validated and relieved and ecstatic — I finally had an answer."
But the relief was short-lived, as Friar quickly realized there was no cure for her condition. "It’s something that you have to try to battle for the rest of your life."
There are, however, options to alleviate some symptoms that come with lipedema, as Friar found out when she began seeing her doctor, Jaime S. Schwartz, M.D., in Beverly Hills, California.
A board-certified plastic surgeon and world-renowned lipedema specialist, Schwartz has dedicated much of his career to raising awareness for fat disorders like lipedema.
He launched Total Lipedema Care to help women like Friar.
"Most people will tell you that the lower half of their body just started growing a lot larger than the upper half, usually during puberty," Schwartz told Fox News Digital.
"It doesn't start as pain, but they start seeing physical changes that don’t really make sense."
Lipedema is usually misdiagnosed as morbid obesity, Schwartz noted.
"In the U.S., many doctors tell women, ‘You're fat, you did this to yourself,’" he said.
MORE THAN HALF THE WORLD'S POPULATION WILL BE OBESE OR OVERWEIGHT BY 2035, SAYS NEW REPORT
But the good news, he said, is that awareness is slowly starting to grow.
"Over the past five years, it's gone from no one knowing about it to a lot of people knowing about it, so it's definitely getting better."
As Schwartz told Friar, he recommends surgery as the best option to relieve lipedema symptoms.
At his practice, Schwartz performs a patented procedure called manual lipedema extraction, which involves a combination of liposuction and the removal of underlying nodules of fat through small incisions.
"When I take the ‘bad tissue’ out, people feel better as soon as the next day," Schwartz said. "That's the only thing that I've seen that works — and I've seen everything that's out there."
Friar ended up having a total of three surgeries — one on the back of her legs, one in the stomach area and one on the front of her legs.
"For me, the surgery was life-changing," Friar said. "I feel it changed the game for me — it extended my life and I gained back probably 75% to 80% of my mobility."
Each surgery required around six weeks of recovery time.
"It isn’t easy, but I would do it 1,000 times over," she said.
One caveat is that some insurance companies have been slow to cover the cost of lipedema surgeries. Friar had to pay out of pocket for the procedures, which can range from $4,000 to $16,000, according to Schwartz's website.
"I was very, very lucky — there are so many women who want the surgery that can't afford it," she said.
In addition to the surgeries, dietary changes have had a big impact on Friar’s quality of life.
"The optimal diet for me is gluten-free and dairy-free, with no added sugars, no processed foods, low salt and very little alcohol," she said.
She also wears medical-grade compression gear at night and lighter-compression leggings during the day.
"It helps alleviate a lot of the inflammation and excess fluid in the body," she said.
Other non-surgical options for relief include exercise and medications or supplements to reduce inflammation.
10 FUNCTIONAL HEALTH PREDICTIONS FOR 2024, ACCORDING TO A DOCTOR AND A WELLNESS EXPERT
As Schwartz told Fox News Digital, Friar’s case was pretty typical of most women’s experiences with lipedema, although he noted her positive mindset.
"A lot of women have had this for so long, and it defeats them emotionally, psychologically and mentally," he said. "But Molly has always had such an amazing outlook and personality."
He added, "Obviously, it's been emotional for her at times, but she never let it defeat her."
Friar said her life now is "like night and day" compared to before.
"Getting a massage for me is now enjoyable," she said through tears. "I can climb to the top of a mountain, and I can walk six miles and not stop."
"It’s like your mobility gets taken away from you, and when you instantly get it back, it's newfound freedom."
Friar’s goal is to increase awareness around this condition, among patients and doctors alike, so other women don’t have to live in shame for years like she did.
CLICK HERE TO SIGN UP FOR OUR HEALTH NEWSLETTER
"It’s something we need to be talking about," she said. "It’s such a visual thing, involving our bodies and how we present ourselves to the world, and it’s something we can’t control."
"I'm willing to shout from the rooftops if I can help even one person recognize the symptoms and be able to help themselves."
For many of Schwartz’s patients, he said, the disease has "destroyed their lives."
"They don't go out, they don't socialize, they're afraid to work or wear certain clothes in public," he said.
Some women can't have their grandchildren sit on their lap or can't hold their spouse's hand because it’s too painful, he said.
"So when they have surgery and they're not in pain, not only do they look different and they're so happy to rediscover their body, but they can even have their dog sit in their lap for the first time," he said.
"It’s a very overwhelming reality for them in a beautiful way," he also said.
It is estimated that around 11% of women are living with lipedema today.
1 year 8 months ago
Health, Obesity, pain-management, lifestyle, Surgery, california, womens-health
Back Pain? Bum Knee? Be Prepared to Wait for a Physical Therapist
At no point along his three-year path to earning a degree in physical therapy has Matthew Lee worried about getting a job.
Being able to make a living off that degree? That’s a different question — and the answer is affecting the supply of physical therapists across the nation: The cost of getting trained is out of proportion to the pay.
At no point along his three-year path to earning a degree in physical therapy has Matthew Lee worried about getting a job.
Being able to make a living off that degree? That’s a different question — and the answer is affecting the supply of physical therapists across the nation: The cost of getting trained is out of proportion to the pay.
“There’s definitely a shortage of PTs. The jobs are there,” said Lee, a student at California State University-Sacramento who is on track to receive his degree in May. “But you may be starting out at $80,000 while carrying up to $200,000 in student debt. It’s a lot to consider.”
As many patients seeking an appointment can attest, the nationwide shortage of PTs is real. According to survey data collected by the American Physical Therapy Association, the job vacancy rate for therapists in outpatient settings last year was 17%.
Wait times are generally long across the nation, as patients tell of waiting weeks or even months for appointments while dealing with ongoing pain or post-surgical rehab. But the crunch is particularly acute in rural areas and places with a high cost of living, like California, which has a lower ratio of therapists to residents — just 57 per 100,000, compared with the national ratio of 72 per 100,000, according to the association.
The reasons are multifold. The industry hasn’t recovered from the mass defection of physical therapists who fled as practices closed during the pandemic. In 2021 alone, more than 22,000 PTs — almost a tenth of the workforce — left their jobs, according to a report by the health data analytics firm Definitive Healthcare.
And just as baby boomers age into a period of heavy use of physical therapy, and covid-delayed procedures like knee and hip replacements are finally scheduled, the economics of physical therapy are shifting. Medicare, whose members make up a significant percentage of many PT practices’ clients, has cut reimbursement rates for four years straight, and the encroachment of private equity firms — with their bottom-line orientation — means many practices aren’t staffing adequately.
According to APTA, 10 companies, including publicly held and private equity-backed firms, now control 20% of the physical therapy market. “What used to be small practices are often being bought up by larger corporate entities, and those corporate entities push productivity and become less satisfying places to work,” said James Gordon, chair of the Division of Biokinesiology and Physical Therapy at the University of Southern California.
There’s a shortage of physical therapists in all settings, including hospitals, clinics, and nursing homes, and it’s likely to continue for the foreseeable future, said Justin Moore, chief executive of the physical therapy association. “Not only do we have to catch up on those shortages, but there are great indicators of increasing demand for physical therapy,” he said.
The association is trying to reduce turnover among therapists, and is lobbying Congress to stop cutting Medicare reimbursement rates. The Centers for Medicare & Medicaid Services plans a 3.4% reduction for 2024 to a key metric that governs pay for physical therapy and other health care services. According to the association, that would bring the cuts to a total of 9% over four years.
Several universities, meanwhile, have ramped up their programs — some by offering virtual classes, a new approach for such a hands-on field — to boost the number of graduates in the coming years.
“But programs can’t just grow overnight,” said Sharon Gorman, interim chair of the physical therapy program at Oakland-based Samuel Merritt University, which focuses on training health care professionals. “Our doctoral accreditation process is very thorough. I have to prove I have the space, the equipment, the clinical sites, the faculty to show that I’m not just trying to take in more tuition dollars.”
All of this also comes at a time when the cost of obtaining a physical therapy doctorate, which typically takes three years of graduate work and is required to practice, is skyrocketing. Student debt has become a major issue, and salaries often aren’t enough to keep therapists in the field.
According to the APTA’s most recent published data, median annual wages range from $88,000 to $101,500. The association said wages either met or fell behind the rate of inflation between 2016 and 2021 in most regions.
A project underway at the University of Iowa aims to give PT students more transparency about tuition and other costs across programs. According to an association report from 2020, at least 80% of recent physical therapy graduates carried educational debt averaging roughly $142,000.
Gordon said USC, in Los Angeles’ urban core, has three PT clinics and 66 therapists on campus, several of whom graduated from the school’s program. “But even with that, it’s a challenge,” he said. “It’s not just hard to find people, but people don’t stay, and the most obvious reason is that they don’t get paid enough relative to the cost of living in this area.”
Fewer therapists plus growing demand equals long waits. When Susan Jones, a Davis, California, resident, experienced pain in her back and neck after slipping on a wet floor in early 2020, she went to her doctor and was referred for physical therapy. About two months later, she said, she finally got an appointment at an outpatient clinic.
“It was almost like the referral got lost. I was going back and forth, asking, ‘What’s going on?’” said Jones, 57. Once scheduled, her first appointment felt rushed, she said, with the therapist saying he could not identify an issue despite her ongoing pain. After one more session, Jones paid out-of-pocket to see a chiropractor. She said she’d be hesitant to try for a physical therapy referral in the future, in part because of the wait.
Universities and PT programs graduate about 12,000 therapists a year, Moore said, and representatives of several schools told KFF Health News they’re studying whether and how to expand. In 2018, USC added a hybrid model in which students learn mostly online, then travel to campus twice a semester for about a week at a time for hands-on instruction and practice.
That bumped USC’s capacity from 100 students a year to 150, and Gordon said many of the hybrid students’ professional skills are indistinguishable from those of students on campus full time.
Natalia Barajas received her PT doctorate from USC last year and was recently hired at a clinic in nearby Norwalk, with a salary of $95,000, a signing bonus, and the opportunity to earn more in incentives.
She’s also managing a lot of debt. Three years of tuition for the USC physical therapy program comes to more than $211,000, and Barajas said she owes $170,000 in student loans.
“If it were about money alone, I probably would have shifted to something else a while ago,” Barajas said. “I’m OK with my salary. I chose to do this. But it might not be the perfect situation for everybody.”
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 8 months ago
Aging, california, Health Industry, States, Medical Education